Table of Contents
Three out of four healthcare executives identify data interoperability as a top priority and for good reason. Secure, real-time data exchange across healthcare systems streamlines processes like claims routing, enhances decision-making by providing timely access to consumer information, and ensures compliance with CMS and ONC requirements.
Is your enterprise ready to harness the power of interoperability? In this blog, we explore how seamless data exchange can optimize operations, drive better outcomes, and position your enterprise for long-term success.
Healthcare Data Interoperability
Data interoperability in healthcare simply refers to the ability of healthcare systems to seamlessly exchange and use health information without disrupting operations or compromising data security. Whether shared within departments or across enterprises, interoperability ensures that critical information moves safely and accurately across the entire care continuum.
Benefits of Data Interoperability in Healthcare
Every healthcare stakeholder has distinct goals when working with data, and data interoperability is vital in helping them achieve these goals. Below are the key benefits of interoperability for healthcare enterprises :
- Elevated Care Experiences : Interoperability allows healthcare enterprises to have seamless access to a member’s complete health history, enabling more informed decision-making and improved care delivery
- Improved Care Coordination : Real-time data sharing between healthcare enterprises reduces redundancy, minimizes the risk of errors, and ensures that all stakeholders have up-to-date, accurate information for better-coordinated and more efficient care delivery.
- Optimized Business Operations : By streamlining data exchanges, interoperability reduces administrative burdens, minimizes manual processes, and enhances overall productivity. This allows healthcare enterprises to focus more on delivering high-quality care and less on operational hurdles.
- Streamlined Claims Processing : Interoperability accelerates claims processing by automating data exchange and reducing manual work. This helps prevent errors and delays, improves cash flow, and makes operations more efficient.
- Better Risk Management : With real-time access to comprehensive and accurate data, healthcare enterprises can more effectively identify, assess, and mitigate potential risks.
- Cost Reduction : Seamless data sharing helps eliminate unnecessary procedures, reduce administrative overhead, and optimize resource utilization, leading to serious cost savings across the healthcare ecosystem.
Barriers to Effective Healthcare Data Exchange

Healthcare enterprises rely on traditional systems such as Health Information Exchanges (HIEs) and Electronic Health Records (EHRs) to manage operational data. However, the varying transmission standards and data formats used by these systems create significant barriers to seamless data exchange between enterprises.
- Legacy Systems: Many healthcare enterprises continue to rely on legacy systems that were not built to meet modern data-sharing requirements. These outdated platforms often lack healthcare API integration and real-time integration capabilities, making seamless data exchange a challenge.
- Disparate Data Formats: Healthcare systems often record and encode the same data in different formats. For example, one system may use a specific code for a diagnosis, while another uses a completely different one. This lack of standardization complicates data sharing and hinders interoperability.
- Stringent Security Regulations: Healthcare data is inherently sensitive and thus requires robust data protection. However, adhering to extensive security regulations while enabling data sharing can create delays. Achieving a balance between securing data and ensuring real-time access remains a critical challenge.
Overcoming Common Barriers To Interoperability
While healthcare interoperability brings substantial advantages to both payers and providers, implementing it often presents various challenges. Below are some effective strategies enterprises use to overcome these barriers and achieve successful interoperability :
Modernize Legacy Systems
Many healthcare enterprises still rely on outdated systems that lack compatibility with modern technologies. Upgrading these systems can be complex, especially when trying to avoid disruptions to daily operations. A phased approach, combining incremental system enhancements with comprehensive staff training can ease the transition, support long-term interoperability, and minimize workflow interruptions.
Prioritize Data Security
Ensuring the security of sensitive healthcare data is a foundational step toward achieving interoperability. Today, enterprises are adopting robust measures such as advanced encryption, role-based access controls, and continuous security monitoring to protect critical healthcare information during data exchange.
These safeguards reduce the risk of breaches, support healthcare data exchange compliance, and foster greater trust among stakeholders.
Adapt to Evolving Regulations
The regulatory landscape in healthcare is constantly evolving, with new data standards and compliance requirements emerging regularly. To ensure ongoing compliance, enterprises must conduct regular audits, update internal policies, and make necessary adjustments to their data exchange frameworks.
A proactive approach to monitoring regulatory shifts not only ensures secure and lawful data exchange but also mitigates the risk of costly compliance violations.
Steps to Implement Healthcare Data Interoperability
To successfully implement healthcare interoperability solutions, enterprises must follow the following key steps:
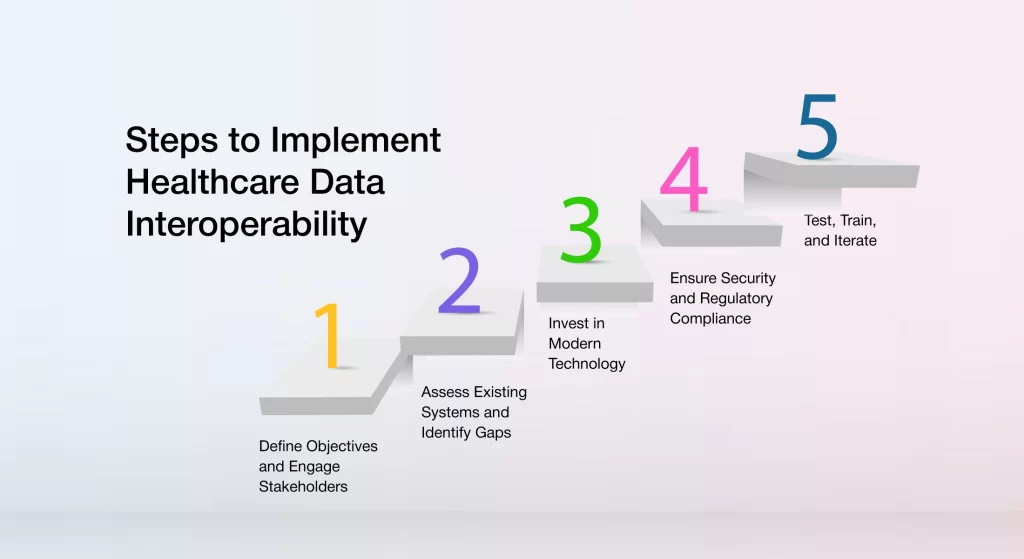
Define Objectives and Engage Stakeholders
The first step in implementing a healthcare interoperability solution is to establish clear goals and engage all key stakeholders like IT teams, payers, and administrative staff from the outset. Involving everyone early in the process ensures alignment on objectives, promotes collaboration, and enables the development of a detailed, unified roadmap. This proactive approach makes sure that all stakeholders are on the same page, laying the groundwork for a successful and coordinated implementation.
Assess Existing Systems and Identify Gaps
Next, enterprises must evaluate their current IT infrastructure and data workflows. This includes reviewing legacy systems, data silos, and any areas where information exchange is inefficient or lacking. By identifying these gaps, enterprises can pinpoint the necessary updates or integrations required to enable seamless data sharing and enhance interoperability across the organization.
Invest in Modern Technology
Achieving true interoperability requires enterprises to move beyond legacy infrastructure and adopt more modern healthcare technologies purpose-built for connected ecosystems. Selecting the right healthcare data interoperability solution designed for payers enables standardized data formats, secure real-time data exchange, and scalable integration across internal systems and external partners.
In practice, cloud-native architectures, scalable APIs, and robust integration platforms play a critical role in unifying disparate systems and improving data accessibility across the enterprise. This foundation not only enhances interoperability but also supports agility, resilience and future-ready digital operations.
Ensure Security and Regulatory Compliance
Safeguarding sensitive healthcare data during exchange is essential for maintaining trust and achieving successful interoperability. Enterprises should always implement robust security measures, such as advanced encryption, role-based access controls, and regular compliance audits, to ensure data integrity.
Additionally, all systems must align with evolving regulatory requirements to protect patient and member privacy.
Test, Train, and Iterate
Before full-scale deployment, enterprises should run pilot programs to assess system performance in real-world scenarios. Along with providing comprehensive training to teams for seamless adoption, it’s crucial to gather and analyze user feedback to pinpoint areas for improvement.
By continuously refining the system based on these insights, enterprises can ensure their sustained effectiveness and adaptability in the long term.
Future Trends in Healthcare Data Interoperability
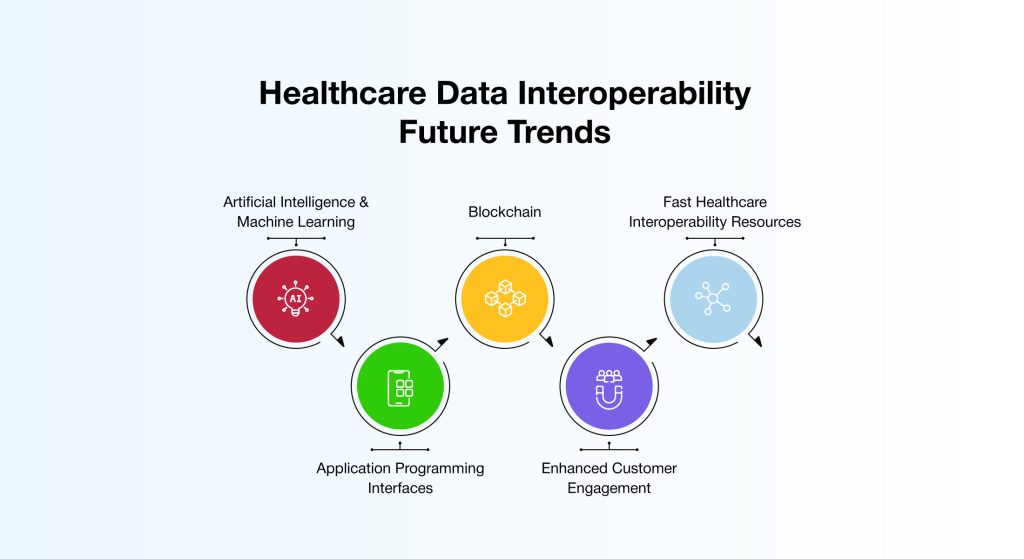
Outdated data exchange methods and persistent data silos continue to hinder efficiency and collaboration across the healthcare landscape. To address these challenges, enterprises are embracing modern, future-ready solutions that promote seamless and secure data sharing.
Below are some of the key innovations and trends shaping the future of healthcare data interoperability:
Artificial Intelligence & Machine Learning
AI and machine learning are transforming how healthcare data is standardized and shared. These technologies automatically classify unstructured EHR data and map it to FHIR standards, enabling real-time decision support.
Furthermore, AI-driven tools are increasingly being used to harmonize and integrate disparate data formats across EHRs, payer systems, and provider networks, minimizing unnecessary intervention and reducing errors.
Blockchain
Blockchain is transforming healthcare data security and interoperability. Emerging applications, such as self-sovereign identity (SSI), empower individuals to directly control access to their health data without relying on intermediaries.
Additionally, federated blockchain networks facilitate secure collaboration between hospitals, insurers, and third-party administrators, ensuring data privacy while enhancing transparency and interoperability.
As the technology evolves, the focus is shifting towards the development of scalable, AI-integrated blockchain networks that enable secure, cross-system data sharing.
Fast Healthcare Interoperability Resources (FHIR)
FHIR is a set of standards designed to simplify and secure healthcare data exchange. By providing a flexible framework for exchanging health information, FHIR facilitates integration across diverse healthcare systems while ensuring compliance with privacy regulations and security protocols.
Application Programming Interfaces (APIs)
The challenge of data silos and isolated systems in healthcare is being addressed through customizable APIs. By establishing specific protocols for data exchange, APIs enable seamless communication between healthcare systems.
Enhanced Customer Engagement
By empowering members with secure, real-time access to their health data, enterprises enable them to actively participate in their care. Advanced consumer portals, AI-driven health insights, and wearable device integrations enable individuals to track their health history, monitor vital signs, and make informed health decisions.
AVIZVA : Redefining The Future of Healthcare Data Interoperability
As healthcare interoperability moves beyond simple data exchange to real-time, compliance-ready connectivity, point integrations are not sufficient anymore. Both payers and providers require a scalable interoperability base that can accommodate regulatory mandates, ecosystem complexity as well as the increasing data velocity.
This is where AVIZVA brings differentiated value. AVIZVA thrives on its 14+ years in health technology integration services across payer, TPA, and PBM ecosystems, helping organizations transition from disparate projects to enterprise-type, forward-looking interoperability by combining real engineering with an appropriately built product ecosystem.
VIZCare Connect sits right at the heart of this ecosystem, an enterprise-grade healthcare data connectivity and interoperability platform for the next generation.
This extraordinary, transformative platform lends its magic to becoming safe, compliant, and predictable in its role for data exchange through every system, partner, and regulator, changing interoperability from being a one-off event to a living, smartly reusing asset that sustains what is later needed for real-time operation and future digital needs.
Key Capabilities That Power Future-Ready Interoperability
- Intelligent Data Orchestration & Synchronization
Today, interoperability requires intelligent, real-time data orchestration over and above simple point integrations to connect the healthcare ecosystem. VIZCare Connect provides this added value by providing automated data synchronization and transformation that ensures accuracy, scale, and operational effectiveness.
Ensures Real-Time Data Synchronization: VIZCare Connect enables real-time data synchronization across internal and external systems, ensuring consistent, reliable data across the healthcare ecosystem. It helps with:
- Continuous synchronization across clearinghouses, providers, PBMs, payers, and regulatory bodies.
- Elimination of data silos and outdated information.
- Accurate, up-to-date data for downstream systems and workflows.
- Support for real-time use cases, including digital experiences and regulatory reporting.
Flexible Data Exchange: To support the diverse and evolving healthcare IT landscape, VIZCare Connect enables flexible data exchange across multiple integration protocols and formats. Supported integration patterns include:
- File-based EDI (Electronic Data Interchange)
- Direct database interfaces
- Modern microservices architectures using JSON
- Asynchronous, event-based integration models for real-time updates and data consistency
Automated Orchestration: VIZCare Connect maintains flexibility with a workflow-driven, automatable data orchestration engine for complex data movement across systems.
In its orchestration, it assists in effortlessly transforming, enriching, and validating data before it is standardized for reaching target systems, ready for business.
Built-in Rules Engine: A native rules engine that enables dynamic data transformation based on business logic and integration essentials, thereby enhancing data consistency, accuracy, and compliance in data exchange across workflows. Key capabilities include:
- Seamless conversion between data formats based on defined business rules.
- Built-in validation to enforce accuracy and compliance.
- Rules embedded directly into interoperability pipelines.
- Rapid adaptability to changing requirements without reengineering integrations.
2. A Comprehensive Healthcare API Suite
As interoperability shifts to real-time, APIs power how healthcare systems connect and operate. VIZCare Connect’s Healthcare API Suite delivers secure, scalable connectivity across the ecosystem.
- Comprehensive API Suite: VIZCare Connect offers a rich suite of 300+ healthcare APIs supporting lookup, read, search, add, and update across core data domains. These APIs simplify integrations across applications, platforms, and partners.
- Built-in Business Logic & Real-World Workflow Support: VIZCare Connect’s APIs embed healthcare-specific business logic to ensure context-aware, operationally meaningful data exchange. This maintains transaction integrity across payer, provider, PBM, and regulatory ecosystems.
- Interoperability & Compliance: VIZCare Connect includes full support for HL7 FHIR APIs to adhere to CMS interoperability mandates and changing legal requirements. Standards-based APIs ensure secure, structured data exchange across ecosystems.
- Preloaded & Continuously Updated Healthcare Industry Data
As interoperability expands, accurate and current reference data is critical to reliable data exchange. VIZCare Connect embeds preloaded, continuously updated healthcare datasets directly into interoperability workflows so that data can be validated, standardized, and enhanced before it is transmitted to downstream systems.
Key datasets include:
- Provider Data (Practitioners & Facilities):
- National Provider Identifiers (NPIs)
- Practitioner taxonomies, specialties, and affiliations
- Practice locations and contact details
- Affiliations & Hospital Privileges
- Medicare & Medicaid Participation Status
- Credentialing & Licensing Information
- Healthcare Code Sets (Standardized Medical, Billing, and Drug Codes):
Supported code sets include:
- CPT for medical services and procedures
- ICD-10 for diagnostic classification
- HCPCS for supplies, equipment, and services
- DRG for case-based reimbursement
- NDC and GPI for pharmacy and drug-related transactions
- Network Data (Payer & Provider Network Information):
- National PPO networks
- Regional PPO networks
- Provider directories and network affiliations
- Pricing, contract, and transparency-related data

Conclusion
Siloed healthcare systems create substantial operational challenges and heighten the risk of errors and security breaches, including unauthorized access to sensitive data. Therefore, data interoperability is crucial not only for meeting regulatory requirements but also for enabling a secure, real-time data exchange environment.
When interoperability is done right, TPAs and PBMs gain more than connectivity. They gain clarity.
AVIZVA helps healthcare organizations move beyond scattered integrations to a more unified, future-ready data ecosystem. With a deep focus on payer, TPA, and PBM workflows, AVIZVA combines healthcare-specific engineering expertise with a purpose-built product ecosystem to simplify data integration, standardize exchange, and enable interoperability that scales with the business.
The future of healthcare data interoperability isn’t about connecting systems once – it’s about building a resilient, compliant, and intelligent data foundation that evolves with the healthcare landscape.
Ready to transform your interoperability strategy? Get in touch with AVIZVA today!

FAQs
1. Why is interoperability critical for healthcare payers and enterprise operations?
Interoperability is critical for healthcare payers and enterprise operations because it enables secure, real-time data exchange across multiple systems and stakeholders. It eliminates data silos and creates a unified view of member, provider, and operational data, allowing payers to operate more efficiently and make better decisions.
For payer organizations in particular, interoperability helps:
- Streamline high-volume processes such as claim process, eligibility, and enrollments.
- Improve coordination across internal teams and external partners.
- Reduce manual work, reprocessing, and data inconsistencies,
Generic integrations often fall short in high-volume, regulation-heavy payer environments. Specialized interoperability solutions address this by:
- Handling large-scale data exchange reliably.
- Supporting CMS and ONC compliance requirements.
- Enabling policy-driven, automated data flows without manual intervention.
Together, these capabilities not only improve day-to-day operations but also create a strong foundation for automation, AI, and predictive analytics—helping payer enterprises scale and remain future-ready.
2. Why do payers require specialized data interoperability solutions?
Payers operate within high-volume, regulation-heavy ecosystems that involve constant data exchange with multiple external entities. Generic integrations often fail to handle this complexity. Specialized interoperability solutions help payers:
- Manage large-scale claims, eligibility, and network data efficiently.
- Support CMS and ONC compliance requirements.
- Enable real-time, policy-driven data exchange without manual intervention.
3. How is interoperability different from integration?
Interoperability and integration, though, are closely related, but they serve different purposes in healthcare technology.
Integration focuses on connecting systems so data can move between them, often through point-to-point interfaces or batch processes. While this enables data exchange, it does not guarantee consistency, context, or real-time usability.
Interoperability, on the other hand, goes beyond connectivity. It ensures that data is not only exchanged but also standardized, understood, and usable across systems in real time. Interoperable systems share a common language, governance, and intelligence layer, enabling seamless collaboration, accurate decision-making, and scalable innovation across the healthcare ecosystem.
4. How can a healthcare organization implement or enable interoperability in its systems?
Successful interoperability necessitates a structured step-by-step approach instead of mere technological upgrades. The path for the organizations is:
- Diagnose existing systems and identify similar data gaps.
- Resort to standards-based platforms (the best of HL7/FHIR and APIs).
- Upgrade legacy systems pointwise.
- Enshrine security, compliance, and governance into data flow.
5. How can organizations ensure healthcare data exchange compliance?
Healthcare data exchange compliance requires security-first, standards-based interoperability frameworks. Organizations can ensure compliance by:
- Using HL7 FHIR and standardized APIs.
- Implementing encryption, access controls, and audit trails.
- Continuously monitoring regulatory updates and conducting audits.
This approach ensures secure, compliant data exchange while remaining adaptable to evolving mandates.

