Table of Contents
Today’s customers expect fast, personalized, and seamless service. They want timely answers, tailored solutions, and consistent experiences across every touchpoint. Yet many insurers continue to struggle with outdated systems, lengthy workflows, and fragmented communication—leading to delays, frustration, and declining consumer satisfaction. And in a highly comp competitive market, these gaps don’t go unnoticed.
This is where AI for insurance companies is redefining what’s possible in healthcare insurance. By integrating solutions for insurance companies into their core business operations, insurers can:
- Automate routine tasks by freeing up teams to focus on high-value, complex cases
- Deliver round-the-clock support across communication channels
- Personalize every customer interaction using real-time insights and behavioral data
AI equips insurers with the tools to overcome operational challenges, enhance efficiency, and meet the evolving expectations of today’s digitally empowered customers.
Ready to explore how AI can elevate your customer experience? Let’s dive in.
Customer Pain Points Insurance Companies Can’t Afford to Ignore
Imagine a customer experiences an unexpected event and turns to their insurance provider for immediate support. But instead of receiving fast, seamless assistance, they’re met with long wait times, multiple handoffs, and limited visibility into what’s happening.
Unfortunately, this isn’t an isolated incident—it’s a common frustration across the U.S. healthcare insurance landscape.
At the heart of the issue is a fragmented experience that no longer meets the expectations of today’s digitally empowered consumers. Let’s explore the most common challenges that stand in the way of delivering a truly seamless, customer-centric healthcare insurance experience.
- Long Wait Times:
Delays in service can significantly impact satisfaction across all consumers including members, brokers, providers, and employers. When individuals are already navigating high-stress situations, long wait times only add friction and diminish confidence in the insurer’s ability to provide timely, dependable support.
- Lack of Personalization:
Today’s consumers expect experiences that reflect their unique needs—whether they’re members seeking care, brokers managing client portfolios, or providers coordinating services. When interactions feel generic or disconnected, it signals a lack of understanding and attention.
Without data-driven personalization, insurers risk losing engagement, reducing satisfaction, and missing opportunities to build stronger, more loyal relationships.
- Communication Gaps And Complex Language:
Clear, timely communication is essential for building trust across all consumer groups. However, many insurers still rely on siloed systems, outdated channels, or jargon-heavy language that creates confusion rather than clarity.
When information is hard to access or harder to understand it leads to frustration, missed follow-ups, and disengagement from members, providers, brokers, and employers alike.
- Managing Diverse Customer Segments:
Healthcare insurers serve a broad range of consumer groups each with unique needs, expectations, and communication preferences. From members and brokers to employers and provider networks, delivering a one-size-fits-all experience simply doesn’t work.
Without tailored engagement strategies and flexible systems, insurers struggle to meet the needs of diverse audiences, resulting in inconsistent service quality and reduced satisfaction across the board.
How AI in Insurance Companies Solves Common Customer Pain Points
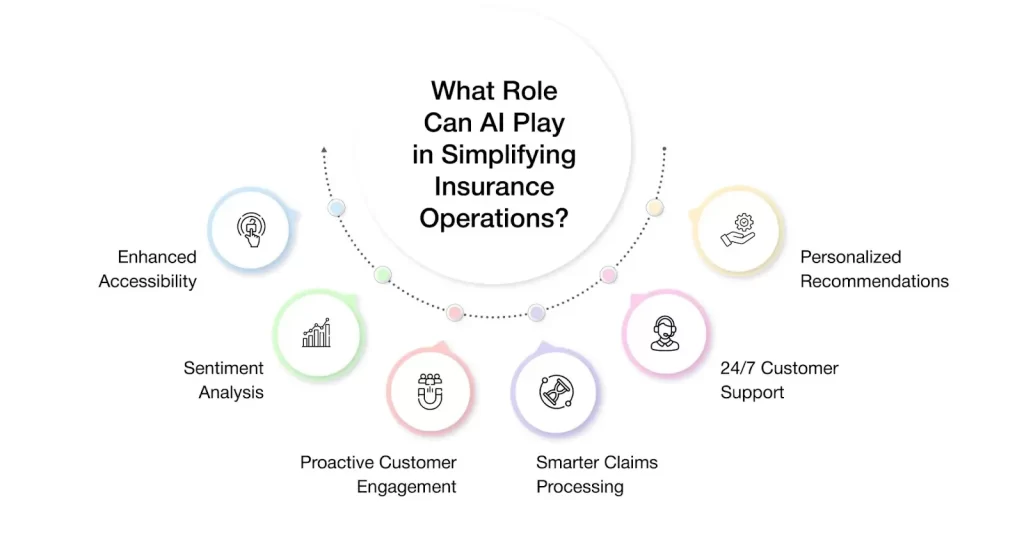
Today’s customers expect fast support, clear communication, and personalized experiences. Yet, many healthcare insurance businesses still struggle with operational delays, overly complex language, and generic interactions, all of which contribute to customer frustration and churn.
This is why AI-driven experiences are gaining momentum across the insurance industry, with AI use cases for insurance companies focused on reducing friction and improving satisfaction at every touchpoint.
1. Delivering Personalized Coverage Recommendations:
No two members have the same healthcare needs and their coverage shouldn’t be identical either.
AI tools for insurance companies enable insurers to analyze individual member data, including historical claims, preferences, demographics, and lifestyle factors, to recommend coverage options tailored to each person’s specific requirements. This level of personalization helps improve plan relevance, enhances member satisfaction, and supports more informed decision-making.
For example, young families might receive plan suggestions that include child education benefits, while retirees could be offered policies with a focus on long-term care and chronic condition support. These personalized recommendations can be delivered seamlessly through the member’s preferred communication channel — whether via SMS, email, or app notifications.
The best AI for health insurance companies helps optimize pricing by assessing individual risk profiles. Instead of applying broad, flat-rate premiums, AI enables more accurate and equitable pricing ensuring members pay a fair rate based on their unique risk factors.
2. Offering Round-The-Clock Consumer Support:
Today’s healthcare consumers from members and providers to brokers and employers expect timely, accurate support at every touchpoint.
AI-powered virtual assistants enable insurers to deliver 24/7 assistance, addressing common queries, guiding consumers through claims and coverage details, and simplifying complex plan information. As these systems continue to learn from interactions, they become faster, smarter, and more accurate over time.
Today, many of these capabilities are powered by AI agents for insurance companies that can interpret user intent, retain conversational context, and guide members, brokers, providers, and employers through eligibility checks, claims tracking, and explanation of benefits within a single frictionless interaction. By combining real-time system access with intelligent orchestration, these AI agents streamline service journeys, reduce handoffs, and deliver faster, more accurate resolution at scale.
Whether it’s a member checking benefits, a provider verifying eligibility, a broker onboarding a client, or an employer managing group plans, insurance companies using AI ensure quick, reliable answers are always available.
3. Enabling Faster & Smarter Claims Processing:
The claims process is often seen as the most critical and frustrating part of the healthcare insurance journey. Delays, manual checks, and a lack of transparency can quickly erode customer trust.
AI solutions for insurance companies help insurers bring greater precision and consistency to this process by automating routine tasks such as document scanning, claim validation, and prioritization. It can flag anomalies for further review while automatically approving straightforward claims, significantly reducing turnaround time and increasing operational efficiency.
For example, an insurer might use AI to instantly process standard outpatient claims, while intelligently routing complex or high-risk cases for manual review. This not only accelerates claim resolution from days to hours but also provides consumers with greater clarity and real-time updates throughout the process — improving both satisfaction and confidence.
4. Driving Proactive Consumer Engagement:
In today’s competitive landscape, healthcare insurance consumers expect more than reactive service they want timely, relevant communication that anticipates their needs.
AI in health insurance companies enables insurers to shift from reactive to proactive engagement by analyzing behavioral data, life events, and usage patterns in real time. It can automatically trigger personalized messages such as wellness tips, renewal reminders, or plan recommendations based on each consumer’s unique context and needs.
For example, when a member adds a new dependent to their plan, AI can proactively suggest a plan upgrade and send a tailored message via their preferred channel. By anticipating needs and delivering value at the right moment, AI helps insurers create more meaningful, consistent touchpoints ultimately improving satisfaction, retention, and lifetime value.
5. Undertaking Real-Time Sentiment Analysis:
Understanding how consumers feel is just as important as knowing what they say yet many insurers miss emotional cues hidden in support interactions. Without insight into sentiment, it’s difficult to identify areas of friction, improve service quality, or prevent churn.
AI-powered sentiment analysis helps insurers monitor and interpret the emotional tone of customer conversations whether through voice calls, chat interactions, or written feedback. It can detect signs of frustration, confusion, or dissatisfaction in real time, enabling proactive improvements in communication, training, and service design.
For example, one insurer used AI to identify a spike in customer frustration during peak claims season. By analyzing sentiment trends, they adjusted messaging, updated FAQs, and re-trained support teams resulting in a noticeable drop in complaints and an increase in customer satisfaction.
6. Enhancing Accessibility & Inclusivity:
Healthcare insurance should be easy to understand and access for everyone. Yet, language barriers and accessibility challenges can prevent many consumers from getting the support they need.
AI helps insurers create more inclusive experiences by offering real-time translation, voice-to-text capabilities, and screen-reader-friendly interfaces. These features ensure that individuals with hearing, vision, or language-related needs can interact with their insurer confidently and independently.
For example, an AI-powered assistant can instantly switch languages for multilingual users or transcribe spoken information for hearing-impaired members enabling seamless access to plan information, support, and services across all channels.
By making insurance more accessible to all, AI supports equity, boosts satisfaction, and ensures no member is left behind.
Despite AI’s Promise, Some Limitations Remain
1. The Need For Human Support:
While AI is highly effective at processing data and handling routine interactions, it lacks the emotional intelligence and ethical reasoning required in more complex or sensitive situations. When members face difficult circumstances — such as navigating a serious diagnosis, appealing a denied claim, or making life-altering coverage decisions — human support is irreplaceable.
In these moments, empathy, reassurance, and sound judgment from a real person are essential to building trust and delivering compassionate care.
2. Limitations Of Off-The-Shelf AI Solutions:
Most ready-made AI tools are not designed to meet the complex, highly regulated needs of the healthcare insurance industry. These solutions often lack the flexibility to adapt to unique workflows, compliance requirements, and data structures specific to each insurer.
As a result, they may fall short in delivering meaningful impact or seamless integration. To unlock AI’s full potential, healthcare insurance enterprises need purpose-built solutions tailored to their operational realities — not one-size-fits-all technology.
3. Concerns Around Data Privacy:
In an era where personal health information is increasingly digitized, data privacy is more important than ever. Consumers are rightfully cautious about how their sensitive information is collected, stored, and used — especially by AI systems. Without clear, transparent data governance and strict compliance with privacy regulations, trust can quickly erode.
Even the most advanced AI solutions will struggle to gain traction if members are uncertain about how their data is being handled. Building and maintaining trust requires not only robust security measures but also clear communication about data use and protection.
4. Integration Challenges With Legacy Systems:
Many healthcare insurance providers still rely on outdated or fragmented legacy systems that were never designed to support modern technologies like AI. Integrating AI solutions with these older infrastructures can be complex, costly, and time-consuming — often requiring extensive customization and workarounds.
These compatibility issues not only slow down AI adoption but also limit its effectiveness, preventing enterprises from realizing the full value AI can deliver.
Given these operational barriers, healthcare insurers need more than just an AI tool — they need a strategic partner who understands their business, customizes solutions to their specific needs, and ensures seamless implementation and adoption.
That’s where AVIZVA steps in. They offer AI-driven solutions that are designed specifically for the healthcare insurance sector — addressing integration challenges, data privacy concerns, and the need for customization. They work alongside insurers at every stage of their transformation journey to ensure AI becomes a sustainable driver of value, efficiency, and improved consumer experiences.
Introducing AVIZVA: AI Solutions for Improving Customer Experience
What if your AI didn’t just respond but understood?
What if every interaction whether from a member, broker, provider, or employer felt informed, consistent, and effortless?
That’s the difference between experimenting with AI and operationalizing it. In healthcare insurance, real value comes from AI that’s purpose-built for complex workflows and delivered through intelligent, human-centered experiences. This is exactly how AVIZVA redefines customer engagement at scale.
AVIZVA is a healthcare technology company that empowers payers, TPAs, and PBMs to enhance care delivery through a comprehensive suite of engineering products and services. With over 14 years of experience in leveraging technology to simplify, optimize, and accelerate care, AVIZVA has become a trusted technology partner to a wide range of healthcare enterprises.
While AVIZVA’s roots are deeply embedded in healthcare insurance, its approach reflects a broader shift in how AI for healthcare companies must be designed domain-aware, compliance-ready, and operationally scalable.
AVIZVA’s healthcare offerings are grouped into two key categories: Engineering Services and its proprietary product suite, VIZCare. Each product within VIZCare is purpose-built to address specific business challenges in healthcare.
To meet the needs of modern insurance consumers, VIZCare AI and VIZCare Xperience offer transformative AI-powered solutions designed to enhance both customer and operational experiences.
VIZCare AI: Enterprise-Grade Healthcare AI for Intelligent Experiences
Most AI platforms can answer questions. Very few understand healthcare insurance.
- Claims logic
- Benefit structures
- Authorization rules
- Network nuances
- Compliance boundaries
These aren’t generic data points, they’re deeply interconnected, high-stakes workflows. And when AI lacks that context, it creates more noise than value.
VIZCare AI was built to solve that exact problem. It is a production-ready, healthcare-specific AI platform where accuracy, context, and control are non-negotiable.
Key Capabilities & Differentiators:
- Deep Healthcare Insurance Understanding: VIZCare AI is trained on real-world healthcare insurance constructs plans, benefits, claims, authorizations, networks, and policies enabling responses and actions that are context-aware, accurate, and domain-relevant across member, broker, provider, employer, and internal use cases.
- Agentic Architecture with End-to-End Functional Coverage: VIZCare AI is built around ready-to-deploy AI agents that directly support healthcare insurance customer service helping teams resolve issues faster, with greater accuracy and consistency.
During interactions, different agents work together behind the scenes to support both members and service teams:
- Service AI Agents assist live calls with real-time guidance, intent understanding, and automatic summaries
- Member AI Agents help customers understand benefits, claims status, and next steps in simple language
- Provider & Operations AI Agents support eligibility checks, authorizations, and service follow-ups without handoffs
These agents, by preserving the context of conversations and workflows, take interactions beyond just Q&A, helping reduce repeated explanations, lessen transfers, and ensure every customer touchpoint feels connected, informed, and efficient.
- Private, Secure & Compliant by Design: Security is not layered on it is foundational.
- Deployed within the customer’s own environment, ensuring full data ownership and control
- Data never leaves the infrastructure; no external model training or data sharing
- Isolated model environments with strict authorization and access enforcement
- Built on enterprise-grade architecture purpose-built for healthcare workloads
- Guaranteed Data Accuracy & Granular Access Control: VIZCare AI enforces compliance-ready design with:
- Role-based and attribute-level access controls
- Secure data handling across sensitive healthcare information
- Privacy-by-design principles that ensure only authorized users can access critical data
This ensures trust, audit readiness, and peace of mind across regulated healthcare ecosystems.
- Flexibility to Build or Adopt: Whether enterprises are looking to start with pre-built conversational AI applications for service agents, members, brokers, providers, and employers, or build fully custom solutions via modular APIs and extensible architecture, VIZCare AI serves as a true AI launchpad for innovation.

VIZCare Xperience: Intelligent Portals That Scale Engagement
One of its leading products is VIZCare Xperience, a suite of AI-powered web and mobile portals built to improve the consumer experience. Designed for payers, TPAs, and PBMs, VIZCare Experience brings all actions and information to the fingertips of the consumers.
VIZCare Experience includes four distinguished products designed for four distinct user groups:
- MemberX: The portal is a one-stop shop for members to manage their coverage, search for benefits, find care, understand claims, and track prior authorizations. While it primarily focuses on enabling ease of self-service, thereby reducing operational workload for enterprises, it also simplifies and enhances interactions with member engagement teams.
- BrokerX: The portal is designed to simplify client acquisition, management & retention for agencies & agents. It brings capabilities to manage the entire lifecycle of clients, covering pre-sales, sales, and post-sales at your fingertips. Some of the most used and high-impact features include quoting and proposals, managing their book of business, accessing commission statements, and gaining ready access to insightful analytics.
- EmployerX: With the needs of employers in mind, the portal is designed to allow effortless management and oversight of employee benefits and usage. Employers can easily manage their group membership, including open enrollment, life change events, member profile information, understanding plan benefits, invoices, and plan performance.
- ProviderX: The portal is designed to cater to both in-network and out-of-network providers, enabling them to understand patients’ benefits, track claims status, payments, and appeals, as well as manage referrals and prior authorizations. It also integrates with the provider empanelment process, offering a comprehensive and unified digital experience for providers.

Conclusion
AI isn’t just a buzzword! It’s a powerful enabler for healthcare insurers looking to transform outdated systems, reduce operational friction, and deliver the fast, personalized, and seamless experiences today’s consumers demand.
From automating routine tasks to personalizing coverage, enhancing accessibility, and proactively engaging customers, AI in insurance companies has the potential to redefine how insurers interact with every consumer.
However, realizing that potential requires more than just technology, it requires the right partner. With purpose-built products like VIZCare Experience and over 14 years of healthcare technology expertise, AVIZVA empowers insurers to implement AI thoughtfully, overcome common barriers, and deliver meaningful, measurable impact.
Ready to bring a smarter, faster, and more personalized experience to your consumers? AVIZVA’s AI-driven solutions are built to make it happen. Get in touch with us today!

FAQs
1. How does AI enhance customer service and communication in insurance companies?
AI improves customer service by offering 24/7 support through virtual assistants and automating responses to common questions. It also simplifies communication by using natural language and preferred channels like apps, texts, or emails.
2. What are the key challenges insurance companies face when adopting AI to improve customer experience?
Healthcare insurers often struggle with outdated systems, strict data privacy rules, and off-the-shelf AI tools that do not fit their workflows. These challenges slow down implementation and limit AI’s full potential.
3. How can AI personalize the insurance buying process for customers?
AI analyzes customer data like past claims, preferences, and life stages to recommend plans that match individual needs. It also customizes communication and pricing, making the buying experience more relevant and engaging.
4. How does AI help insurance companies handle claims more efficiently and accurately?
AI speeds up claims by scanning documents, verifying details, and flagging suspicious activity. It reduces manual errors and shortens processing time, improving both accuracy and transparency.
5. What impact does AI have on customer satisfaction and loyalty in the insurance industry?
By offering faster service, clearer answers, and personalized plans, AI helps insurers build trust and satisfaction. Customers feel understood and supported, which increases loyalty and retention.
6. What are the ethical concerns around using AI in customer service, especially in the insurance sector?
Ethical concerns include data privacy, transparency in decision-making, and the risk of over-automation. Customers need to know how their data is used, and sensitive situations still require human involvement.
7. How can AI help insurance agents in their daily operations?
AI supports insurance agents by reducing manual effort and improving decision confidence. It helps agents:
- Provides instant, context-aware insights on coverage, claims processes, and authorizations.
- Assisted by AI, it cuts down on time for manual data lookup through summaries and recommendations.
- Makes the reply more accurate by using healthcare insurance knowledge domain-trained intelligence.
- Directs agents on how to take the next steps of a complicated workflow, so they can solve queries quickly.
- Through voice, chat, and internal systems, it helps in providing uniform answers, leading to a better quality of service.
- By doing routine, repetitive interactions, it saves time for carrying out high-value tasks.
- Learning eventually, the AI adjusts from real interactions, thus continuing in accuracy and learning support.
This translates into quicker problem solving, enhanced productivity, and better service consistency.
8. What are some practical AI use cases for insurance companies?
AI is commonly used to automate service inquiries and personalize consumer interactions at scale. It also enables proactive outreach through timely alerts and recommendations, and analyzes interaction sentiment to improve service quality. Together, these use cases drive efficiency while improving overall customer experience.
9. Is AI replacing human insurance agents?
No. AI complements human agents rather than replacing them. It handles high-volume, repetitive requests and information retrieval, while agents focus on complex scenarios, exceptions, and situations that require empathy or decision-making. This partnership improves both productivity and service consistency.
10. How secure is AI technology in handling sensitive insurance data?
When designed for healthcare insurance, AI platforms are built with security and compliance at the core. They operate within controlled environments, apply role-based access controls, and follow privacy-by-design principles aligned with regulatory requirements. This ensures sensitive insurance data remains protected, auditable, and trustworthy.

