As the healthcare insurance landscape undergoes a rapid digital transformation, enterprises face the critical challenge of navigating shifting consumer expectations.
From members and providers to brokers and employers, every healthcare consumer now demands a digital experience that is seamless, personalized, and intelligent. To meet these rising demands, healthcare enterprises must integrate future-ready AI in customer experience capabilities into their existing experience portals and applications.
In this blog, we explore the top five AI use cases in customer experience, highlighting how technologies are enhancing the healthcare insurance journey for consumers.
Top 5 Ways In Which AI Is Elevating Consumer Experience In Healthcare Insurance
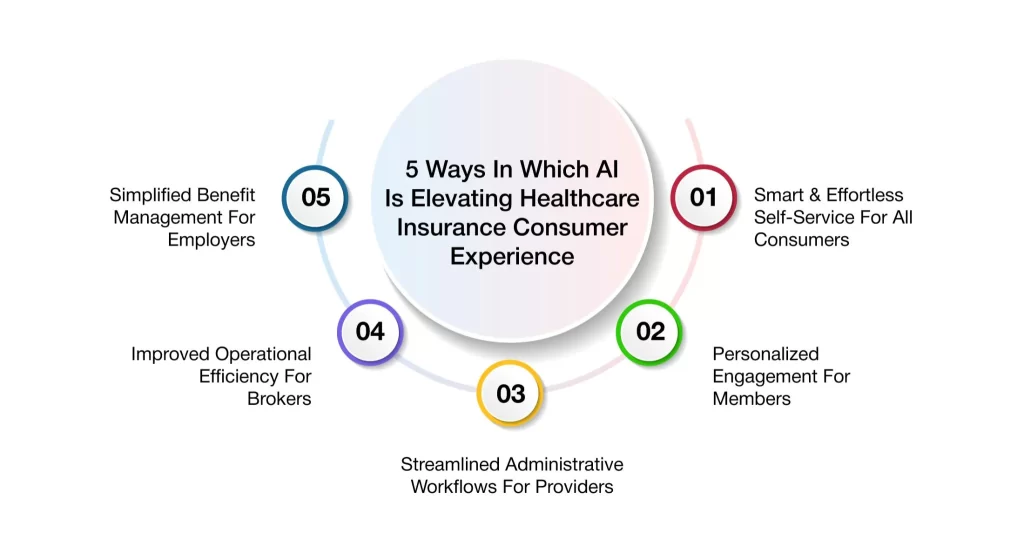
1. Smart & Effortless Self-Service For All Consumers
Navigating healthcare insurance shouldn’t feel like decoding a puzzle while on hold for 45 minutes. Yet, for many consumers, that remains the norm. Outdated IVRs, clunky portals, and inflexible chatbots are hindering the experience in an era when convenience is king.
To meet the expectations of the modern healthcare consumer, forward-thinking insurers are ushering in a new era of intelligent, AI-powered self-service. These aren’t your average bots. We’re talking about AI assistants with a deep understanding of healthcare, capable of engaging in natural, human-like conversations—anytime, anywhere.
Here’s what makes them revolutionary :
- 24/7 Omnichannel Access: Whether it’s through a mobile app, website, or voice assistant—support is always just a message away.
- Healthcare-Specific Intelligence: From plan benefits to prior authorizations, these AI copilots are trained to speak the complex language of healthcare.
- Conversational & Human-like: Powered by advanced natural language processing, interactions feel intuitive, not robotic.
- Action-Oriented Help: Think beyond FAQs—these assistants actually assist consumers in resolving tasks, not just reading about them.
Collectively, these capabilities demonstrate how AI enhances customer experience in healthcare; shifting from rigid, transactional interactions to intelligent, conversational and always-on engagement that delivers both convenience and operational efficiency.
2. Personalized Engagement For Members
In a system as complex as healthcare, one-size-fits-all is ineffective; this is where AI-driven customer experience becomes a true differentiator
Every member has unique health needs and preferences and they expect health insurance enterprises to recognize and reflect that. Today’s members demand more than just coverage; they want meaningful, personalized engagement that reflects who they are and what they need.
To meet these expectations, enterprises are harnessing the power of AI-powered customer insights into their member experience platforms. These next-gen platforms tap into health records, claims history, lifestyle data, and real-time behaviors to create a 360° view of the member—unlocking moments that matter.
Here’s how it works:
- Tailored Plan Recommendations: AI analyzes individual usage and preferences to guide members toward the most suitable plans during renewals or life events.
- Proactive Health Nudges: Automated reminders for screenings, refills, or preventive care—delivered at the right time, via the right channel.
- Custom Communication Journeys: Whether it’s email, SMS, app notifications, or a chatbot ping—messages are context-aware and tailored to each member.
This shift from transactional to relational engagement isn’t just smart—it’s essential. And the result? Higher satisfaction, improved health outcomes, and stronger member retention.
3. Streamlined Administrative Workflows For Providers
In the complex world of healthcare, providers are often torn between delivering quality care and managing an increasing workload of administrative tasks.
Administrative demands such as mountains of paperwork, endless eligibility checks, and repetitive claims follow-ups from health insurance enterprises continue to consume a considerable amount of providers’ time, reducing their ability to prioritize the delivery of high-quality care.
To address this challenge, healthcare insurance enterprises are integrating AI-driven automation into their provider experience platforms. These intelligent platforms are designed to reduce friction across administrative workflows, positioning AI as an operational differentiator that enhances customer experience while freeing up capacity to focus on what truly matters – care.
Here’s how AI is transforming provider operations:
- Real-Time Eligibility Verification: Instant checks reduce delays and eliminate the need for back-and-forth communication.
- Automated Prior Authorizations: Speed up approvals with minimal manual intervention, reducing frustration and treatment delays.
- Intelligent Claims Tracking: AI in customer experience monitors claim status in real time, flags anomalies, and provides actionable insights.
4. Improved Operational Efficiency For Brokers
Brokers are the lifeblood of health insurance distribution—trusted advisors who help individuals and employer groups navigate the maze of plans, pricing, and policies. However, routine manual tasks often consume their bandwidth, diverting focus away from the strategic counsel and personalized service that clients rely on.
To solve this, healthcare insurance enterprises are integrating AI-enabled automation into their broker experience platforms. By streamlining complex tasks such as quoting, plan comparison, and enrollment, these intelligent platforms empower brokers to work more efficiently, make faster decisions, and deliver greater value.
The result? Less time spent on paperwork, more time building relationships and closing deals with precision, speed, and confidence.
5. Simplified Benefit Management For Employers
Employers play a pivotal role in administering health insurance benefits and promoting the overall well-being of their workforce. Yet, managing these benefits—while catering to a diverse employee base and meeting ever-evolving compliance demands—remains a complex, resource-heavy endeavor.
To simplify this landscape, healthcare insurance enterprises are transforming customer experience with AI and automation through their employer experience platforms. These advanced platforms optimize benefits administration by automating enrollment workflows, providing real-time analytics on benefits utilization, ensuring regulatory compliance, and facilitating personalized communication.
As a result, employers are empowered to manage health plans more efficiently while enhancing overall employee satisfaction.
Turn AI Use Cases into Action with AVIZVA’s Expertise
By 2026, consumer experience will no longer be defined by access alone; anticipation, clarity, and continuity will set leaders apart.
AI-driven experiences are raising the bar across industries, including insurance, where consumers now expect systems to be less static portals and more intelligent digital companions. This evolution is the face of tomorrow’s AI-powered customer experience where the AI anticipates intent, makes decisions simpler, and proactively drives action.
AI in consumer experiences is more about predicting intent, simplifying decisions, and proactively driving actions rather than just reacting quickly.
VIZCare Xperience MemberX translates the top AI use cases in consumer experience into a unified, intelligent engagement ecosystem, designed to deliver relevance, personalization, and consistency at every interaction. Here’s how it helps:
- Intelligent AI-Driven Assistance and Insights
Real-time intent and context understanding is a core AI use case in consumer experience. VIZCare AI powers intelligent assistance that adapts guidance based on what users need and when they need it.
- Conversational support across chat, voice, and text
- Plain-language explanations of coverage, policies, and updates
- Personalized alerts, reminders, and proactive nudges
- Insights that adapt continuously based on behavior and engagement
With VIZCare AI embedded into the experience layer along with an assistant provided, AI-as-chaperone must become imaginative, behavioral, and hands-on to raise industry standards in digital health by 2026.
- Full Self-Service Capabilities
AI-powered self-service is a cornerstone of modern consumer experience. Empowered users expect fast, frictionless access without relying on support channels.
With VIZCare Xperience, self-service means:
- Unified visibility into benefits, coverage, and activity
- Real-time tracking with AI-assisted summaries
- Digital access to documents and key information
- Anytime availability across web and mobile
- Seamless Experience Across All Channels
Another critical AI use case is omnichannel continuity. Consumers expect to move across platforms without losing context or repeating themselves.
MemberX delivers:
- Consistent engagement across web, mobile, chat, and messaging
- Smooth handoffs from AI to live assistance when needed
- Preserved conversation history across channels
- Always-on access with contextual continuity
- Tailored Campaigns to Drive Better Health Outcomes
AI transforms consumer experience from transacting nothing into offering tailored, predictive engagement. No longer concerned with responding to requests, AI begins to help with meaningful actions. Features include:
- Personalized education and engagement campaigns
- Targeting based on behavior, demographics, and usage patterns
- Multi-channel outreach via SMS, email, and in-app messaging
- Real-time monitoring of engagement and effectiveness
- Making Healthcare Decisions Easier and More Transparent
Decision clarity is a defining AI use case in consumer experience. When information is simplified and contextualized, confidence follows.
The platform supports clarity through:
- Intelligent search and guided discovery
- Clear breakdowns of coverage and options
- On-demand access to virtual services
- Transparent insights that remove ambiguity
- Driving Adoption and Sustained Engagement
Even the most sophisticated AI experience gains value only when it is consistently utilized. Proactive AI guidance and intuitive design together will control long-term engagement in a 2026 makeover.
MemberX focuses on:
- Clean, modern UX with minimal learning curves
- Guided onboarding and contextual assistance
- Smart nudges that encourage repeat engagement
- Integrated support to avoid dead ends

Engagement That Extends Beyond Members
AI-led consumer experience extends beyond members into the wider ecosystem. VIZCare Xperience reflects this interconnected reality through experience gateways that support every stakeholder touchpoint:
- BrokerX : Empowering Brokers with Full Control, Insight, and Efficiency for Better Client Acquisition and Retention
- EmployerX : Enable Employers To Manage Group Memberships & Benefits Utilization With Ease
- ProviderX providing Tools, Insights, and Transparency at Every Stage of Interaction with Payers to providers
To understand how each platform contributes to this connected experience and how AVIZVA’s engineering services help tailor, integrate, and optimize these solutions for real-world environments, explore VIZCare Xperience in action.
Conclusion
It’s clear: Today’s healthcare customers want more than just answers. They want speed, clarity, and a personal touch. That’s where AI in customer experience truly shines. It helps insurers move from slow, disconnected processes to real-time, meaningful experiences.
Imagine a world where members get the right plan suggestion before they even ask – an emerging AI customer experience example already reshaping insurance.
That’s not a dream, it’s already happening.
At AVIZVA, we don’t just talk about AI—we build it into real solutions that work for real people. Our platforms: VIZCare Xperience and AI are designed keeping your customers in mind. No matter where you are in your journey, we’re here to help.
Wondering whether AI can improve your customer experience? AVIZVA makes it practical and possible. Let’s chat!

FAQs
1. How does AI help in healthcare customer experience?
AI makes healthcare service faster, simpler, and more personal. It allows members to check claims, get policy answers, and complete tasks instantly—without waiting on hold. AI also offers tailored reminders, explains complex terms in plain language, and provides 24/7 self-service across channels.
2. What are the main ways AI is used in customer experience?
AI enhances customer experience by enabling instant self-service, delivering personalized responses, and automating routine tasks. It powers chatbots, virtual assistants, and smart search tools, helping users get clear answers anytime. For support teams, AI provides real-time suggestions, auto-notes, and full customer context—leading to faster, more satisfying interactions.
3. Do industries use AI to make the customer experience better?
Yes, many industries—from healthcare and insurance to retail and banking—leverage AI to deliver faster, smarter, and more personalized customer experiences. AI helps automate support, offer 24/7 self-service, and anticipate customer needs with data-driven insights. The result? Quicker resolutions, happier customers, and stronger brand loyalty.
4. Are AI-powered customer experiences safe and follow rules?
Yes. When done right, AI can be secure and comply with industry regulations, such as HIPAA. Platforms like AVIZVA’s Co-Pilot are built with safety and fairness in mind.
5. What makes AVIZVA a strong partner for AI in customer experience?
AVIZVA combines deep healthcare domain expertise with cutting-edge AI engineering to deliver smart, scalable, and secure customer experience solutions. With products like VIZCare AI and VIZCare Empower, AVIZVA is helping enterprises transform how they engage with members, providers, brokers, and employers—offering intelligent self-service, contextual support, and real-time automation.
6. What role does generative AI play in modern customer experience?
Generative AI enables more intuitive, conversational, and proactive digital experiences across insurance touchpoints. It helps enterprises:
- Deliver plain-language explanations of benefits, coverage, and updates.
- Power conversational self-service across chat and voice.
- Anticipate intent and guide next-best actions in real-time.
- Proactively surfaces relevant options, reminders, or alerts.
7. How does AI help reduce operational costs in customer service?
AI reduces costs by automating high-volume, repetitive interactions while improving resolution speed. For healthcare insurers, this includes:
- Deflecting routine inquiries through intelligent self-service.
- Automating eligibility checks, status updates, and follow-ups.
- Reducing manual effort while maintaining consistent service quality.
8. What are the top AI-powered customer experience use cases?
AI is increasingly used to make interactions easier, faster, and less frustrating across insurance journeys. The most common use cases include:
- 24/7 AI Customer Support: AI chat and voice assistants handle common queries like policy details, claim status, coverage checks, and payment reminders, anytime, without waiting for an agent.
- Faster Claims Assistance: AI walks customers through claim initiation, document submission, and status tracking, reducing confusion and cutting resolution time.
- Intelligent Call & Ticket Routing: AI understands intent and routes queries to the right team or agent, improving first-contact resolution.
- Real-Time Agent Support: AI supports agents with real-time customer context, recommended responses, and next best actions during live interactions.
- Sentiment & Experience Analysis: AI monitors conversations to detect frustration or dissatisfaction, helping teams intervene before issues escalate.
