Table of Contents
| TL;DR 1. Business Imperative: Automation alone can’t keep pace with real-time, enterprise healthcare complexity. 2. Problem: Static workflows break at the “last mile” during exceptions, data changes, and compliance shifts. 3. Solution: Intelligent orchestration powered by VIZCare products helps align data, decisions, and execution in real-time. 4. Key Outcome: Faster decisions, built-in compliance, and resilient operations at enterprise scale. |
The digital health ecosystem is undergoing a rapid transformation, and enterprise healthcare organizations particularly payers, TPAs, and PBMs are experiencing growing operational strain. Increasing regulatory complexity, rising service expectations, and expanding data ecosystems are exposing the limitations of traditional efficiency strategies.
For years, operational optimization in healthcare focused on reducing human effort through workflow automation. While technologies such as Robotic Process Automation and rule-based automation delivered measurable productivity improvements, they were designed to execute isolated tasks not to manage interconnected enterprise processes. As healthcare operations grew more complex, these task-driven solutions began creating fragmented workflows, limited adaptability, and increasing dependency on manual intervention to resolve exceptions.
Today, many organizations are experiencing what can be described as last-mile automation failures where automated tasks operate independently but fail to collaborate, synchronize data, or adapt to changing business rules and regulatory requirements. The result is operational inefficiency disguised as automation.
To overcome this challenge, healthcare enterprises must shift from automation to intelligent orchestration, an approach that unifies data, workflows, and AI-driven decision-making across systems, departments, and stakeholders. Intelligent orchestration enables organizations to move beyond executing tasks to coordinating outcomes, ensuring processes remain adaptive, compliant, and context-aware across the healthcare value chain.
In this blog, we explore why automation alone is no longer sufficient for enterprise healthcare operations and examine how VIZCare enables adaptive, end-to-end orchestration designed to meet the demands of modern healthcare ecosystems.
Decoding the “Last Mile” Failure of Legacy Automation
Most enterprise healthcare leaders are now confronting what can be described as the “last-mile” failure of automation, a persistent challenge that remains unresolved despite years of investment in workflow automation technologies.
What is the “last mile” problem?
Healthcare enterprises have extensively adopted RPA and BPM platforms to automate repetitive, high-volume operational tasks such as data entry, validations, and transaction updates. These solutions perform effectively when workflows are predictable and rules remain stable.
The challenge emerges at the final stage of operational workflows, the “last mile”, where cases require coordination across multiple systems, real-time decision-making, or human-level judgment. Traditional automation frameworks are not designed to manage these complexities.
Consider a claims processing scenario. A claim may successfully pass initial automated validation checks but encounter friction when it requires coordination across multiple payers, real-time eligibility updates, or interpretation of evolving policy guidelines. When information is incomplete, exceptions arise, or regulatory rules shift, static workflows lack the intelligence to adapt. As a result, these cases are redirected to manual processing teams introducing delays, increasing administrative costs, and creating repetitive rework.
| Takeaway: The process doesn’t fail at the beginning; it fails at the final step. |
Why Traditional Automation Is Stalling:
- Disintegrated Data: When claims data, provider contracts, eligibility information, and compliance records exists across disconnected systems, automation cannot reconcile inconsistencies in real time. As data falls out of sync, exceptions multiply, forcing manual intervention and amplifying errors at scale.
- Uncoordinated Workflows: Automation often optimizes individual tasks but fails to coordinate end-to-end processes across departments. When functions such as claims processing, compliance validation, and provider operations in silos, workflow handoffs become inefficient, operational visibility diminishes, and issues surface too late; creating systemic slowdowns.
- Compliance Gaps: Legacy automation platforms struggle to keep pace with evolving regulatory mandates. Compliance checks are often reactive, reliant on static rule libraries, or applied after workflow completion exposing organizations to penalties, audit risk, and reputational exposure.
Simply deploying additional bots or expanding rule sets cannot resolve the last-mile problem. Addressing this challenge requires a fundamentally different approach, one that dynamically coordinates workflows across systems, intelligently adapts to changing business conditions, and continuously aligns operations with regulatory and operational requirements.
To move forward, enterprise healthcare organizations must adopt an intelligent orchestration model that is designed to unify data, workflows, and AI-driven decision-making across the entire operational ecosystem.
The Shift to Intelligent Orchestration in Enterprise Healthcare
As traditional automation approaches its functional limits, enterprise healthcare organizations are transitioning toward a more adaptive and resilient operating model: AI-powered orchestration in healthcare that synchronizes data, decisions, and execution in real time.
This shift represents a fundamental evolution in how healthcare operations are managed. Instead of automating isolated tasks, orchestration connects entire workflows ensuring processes remain responsive, compliant, and aligned across complex healthcare ecosystems.
What Intelligent Orchestration Really Means
In enterprise healthcare, intelligent orchestration enables organizations to :
- Coordinate workflows across operations domains spanning claims processing, provider management, member services, compliance operations and other critical functions in real-time.
- Continuously respond to data changes by dynamically adapting workflows to reflect eligibility updates, regulatory changes, provider information updates, and evolving member activity
- Use AI-driven insights and rules-based logic to guide workflows at the moment decisions are required, reducing exceptions and accelerating resolution..
- Combine machine-driven execution with human oversight for judgment-intensive, sensitive, or exception-based scenarios
Traditional automation typically focuses on sequencing predefined tasks. Instead of asking “What task runs next?” orchestration asks, “What action creates the best outcome right now?
Why Static Workflows Fail at Enterprise Scale
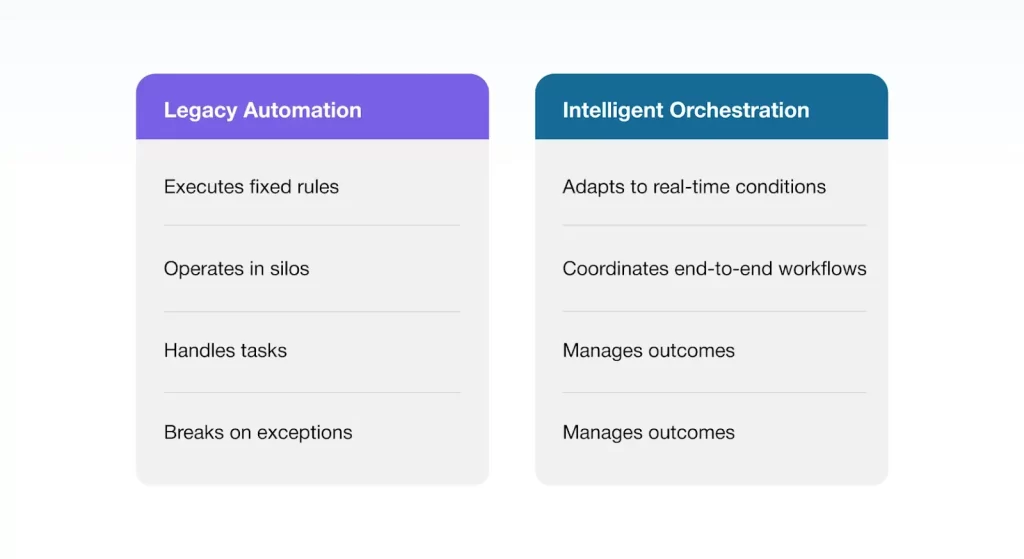
High-Impact Use Cases for Payers
Intelligent orchestration unlocks operational capabilities that traditional, task-based automation cannot support at enterprise scale. By synchronising data, workflows and AI-driven insights, payers can deliver adaptive, real-time operations across critical business functions.
- Real-time claims adjudication that adapts to eligibility and benefits changes
Intelligent orchestration enables claims processing systems to dynamically respond to eligibility or benefits updates as they occur.
For example: when a claim is submitted following a same-day eligibility modification, the system automatically revalidates benefits coverage in real time ensuring accurate adjudication without manual intervention, rework, or processing delays. - Predictive care management triggered by live risk signals
Orchestrated intelligence enables early intervention by monitoring behavioral patterns and service utilization trends.
For instance, if a member’s care usage or engagement activity shifts unexpectedly, the system can instantly identify risk indicators and trigger care management workflow initiating outreach or clinical interventions without waiting for scheduled reviews. - Integrated compliance workflows with built-in audit visibility
Intelligent orchestration ensures regulatory compliance is continuously enforced across operational processes. When regulatory requirements such as CMS guideline updates are introduced, orchestration engines can apply updated rules across workflows immediately. At the same time, every operational step is automatically recorded, creating built-in audit trails and ensuring continuous compliance and reporting readiness
By combining AI with orchestration, healthcare organizations transition from reactive task execution to adaptive enterprise operations. This evolution enables orchestrated automation within healthcare environments to become more resilient, compliant, and scalable while improving both operational efficiency and stakeholder experience.
The Benefits of Intelligent Orchestration in Enterprise Healthcare
Intelligent orchestration, enables healthcare organizations to establish a unified, enterprise-wide orchestration strategy that delivers measurable operational and business outcomes. Key benefits include:
- Improved Operational Efficiency: Unlike traditional automation that optimizes workflows in isolation, intelligent orchestration connects processes across systems, teams and operational functions.
- Reduces manual handoffs across departments
- Eliminates rework caused by disconnected processes
- Keeps operations moving even when conditions change.
Example: A claim is submitted with incomplete provider information. Instead of halting the process, the orchestration engine automatically requests the missing data, routes the case to the appropriate stakeholder, and resumes processing once the update is received.
The result is smoother execution across complex enterprise environments.
- Faster, More Accurate Decision-Making: With real-time data availability and AI-based coordination, organizations no longer need to delay decisions while waiting for batch processing or downstream validations.
- Actions dynamically adapt to live data changes
- Exceptions are identified and resolved earlier in the workflow
- Errors caused by outdated rules or incomplete context are minimized
Example: A member’s utilization pattern shifts unexpectedly, indicating higher clinical or financial risk. The system detects this change in real-time and immediately triggers the appropriate workflow alerting care teams or adjusting next steps immediately.
This directly improves turnaround times while strengthening decision confidence across operational teams.
- Built-In Transparency and Compliance: Intelligent orchestration embeds governance directly into operational execution, ensuring compliance is continuously enforced rather than applied retroactively.
- Every action is automatically tracked and documented
- Policies and regulatory requirements are enforced during workflows execution
- Audit visibility is built into processes by design
Example: As a claim progresses through review stages, regulatory checks are applied automatically at each checkpoint. Every action is logged, and approvals are recorded in real-time. This automatically creates audit trails, eliminating last-minute compliance reviews and reducing risk.
This approach reduces compliance risk while lowering administrative effort.
- Enterprise-Grade Scalability: As operational complexity and transaction volumes grow, orchestration provides a flexible foundation that scales without disrupting existing workflows.
- New workflows can be introduced without impacting existing processes
- Operations adapt seamlessly to regulatory and business change
- Systems can support increased volumes and process variability without performance degradation
Example: When a new regulatory mandate or payer requirement is introduced, organizations can update rules centrally. Workflows automatically adjust across the enterprise, enabling rapid compliance and business scalability without redesigning core processes.
Collectively, these benefits translate into reduced operational costs, enhanced stakeholder experience, and improved regulatory readiness, three strategic priorities that define success for enterprise healthcare leadership in today’s evolving ecosystem.
VIZCare Suite Enabling Intelligent Orchestration at Scale
Automation is everywhere. Orchestration is not.
Enterprise healthcare organizations don’t have an automation problem, they have an orchestration gap.
Closing this gap takes more than tools. True orchestration happens when data connectivity, decision intelligence, and execution layers work together continuously and in real time. Built by AVIZVA, the VIZCare product suite delivers exactly that, serving as one of the most comprehensive intelligent orchestration platforms for healthcare in 2026 and beyond.
Here’s how.
VIZCare Connect: Powering Real-Time Connectivity and Orchestration
Intelligent orchestration depends on one critical foundation: real-time, reliable data across the enterprise. VIZCare Connect provides this foundation by orchestrating data movement across systems powered by intelligence from VIZCare AI.
- Real-Time Data Synchronization: Keeps data continuously updated across internal systems and external stakeholders such as clearinghouses, PBMs, and regulatory bodies. This eliminates data silos and ensures every workflow is operated considering the most current information.
- Flexible Data Exchange: Interfaces with diverse integration protocols and formats, including file-based EDIs to direct database connections, microservices with JSON, and event-driven architectures, among others. It pools systems of different, varied designs without having to redesign the existing infrastructure.
- Automated Orchestration: Uses a configurable, workflow-driven orchestration engine to automate complex data flows across systems. Data is transformed, enriched, and validated automatically, removing manual intervention and reducing delays.
- Built-In Rules Engine: Within the dynamic data transfer, the rules engine handles data transformation based on integration and operational demands. It helps render uniform and structured data handling across the entire enterprise workflow.
How VIZCare AI powers VIZCare Connect:
While Connect ensures the plumbing of enterprise healthcare data, VIZCare AI gives it intelligence.
VIZCare Xperience: Orchestrating Intelligent, AI-Driven Consumer Experiences
Orchestration of intelligence rolls out from enterprise to consumer as real-time workflows are transformed nutritiously through AI into digital experiences. With consumer experience at the core, it delivers guided, self-service journeys powered by live data, ensuring accurate information, seamless interactions, and reduced service friction.
Portal Experiences Tailored for Every Consumer Group
MemberX: Simplifying Member Engagement & Health Navigation
MemberX is a unified member portal that places coverage, benefits, claims tracking, care search, and plan actions at members’ fingertips. It empowers members with self-service tools while reducing support load on enterprise teams.
- Instant access to coverage details, eligibility, and benefit summaries.
- Real-time claims and prior authorization tracking.
- Conversational AI that answers questions in plain language.
- Smart document summaries for policies and EOBs.
- Personalized health insights and reminder nudges.
- Multi-channel continuity across web, mobile, and messaging.
BrokerX: Advancing Broker Productivity & Client Success
BrokerX empowers brokers and agents with tools that streamline client acquisition, retention, and relationship management:
- Manage book of business with real-time access to policies and commissions.
- Generate and manage quotes, proposals, and renewals.
- Gain insights into utilization trends, churn risks, and cross-sell opportunities.
- AI-driven support for faster responses and personalized client servicing.
- Seamless payer, broker, and client communication and collaboration for faster resolutions.
EmployerX: Empowering Employers With Benefits Oversight & Analytics
EmployerX helps employers manage group benefits and employee engagement with simplicity and clarity:
- Group membership management, including open enrollment and life event updates.
- Real-time visibility into benefits usage and invoices.
- Smart analytics on utilization and cost trends.
- AI-guided renewal recommendations and proactive alerts.
- Integrated communication with brokers and payers for aligned decision-making.
ProviderX: Elevating Provider Collaboration & Efficiency
ProviderX brings transparency and tools to healthcare providers, enabling them to access essential data and manage key workflows:
- Instant eligibility & benefits verification.
- Digital submission and tracking of claims, authorizations, and appeals.
- Price and reimbursement estimates with clear breakdowns.
- Smart clinical insights from health history summaries.
- Provider onboarding, credentialing, and network management – all within the portal.
How VIZCare AI Powers Xperience Across Portals
Behind every experience in Xperience is VIZCare AI: the intelligence layer that analyzes context, behavior, and workflows to make interactions predictive, responsive, and personalized. It drives:
- Context-aware assistance that anticipates needs.
- Proactive outreach that nudges users toward timely actions.
- Natural language understanding for intuitive conversations.
- Adaptive personalization is unique to each consumer group.
By embedding AI into every layer of Xperience, the suite doesn’t just deliver information; it guides users to outcomes faster, reduces friction, and enhances satisfaction across all stakeholders.
VIZCare Empower: AI-Driven Service Orchestration for Enterprise Healthcare
VIZCare Empower uplifts human-assisted service with AI-guided assistance and live orchestration, ensuring every interaction becomes competent and consistent. This service execution layer combines orchestrated intelligence to help teams resolve issues more promptly and precisely.
How VIZCare Empower Elevates Consumer Servicing
- Omnichannel Consistency: Enables seamless service across voice, text, chat, and IVR, ensuring consistent interactions.
- Single Pane of Glass for Service Teams: The user is given access to a single-space dashboard to manage, ensure appropriate upkeeping, update member provider, broker, and employer information, with no need for system gap navigation.
- AI-Powered Real-Time Assistance: Uses VIZCare AI to deliver live guidance, next-best-action prompts, knowledge base access, and intelligent recommendations during interactions.
- Real-Time Eligibility and Data Checks: Real-time validation during the call ensures accuracy and confidence throughout service delivery.
- Managed Tasks and Next Steps: Generation and allocation of follow-up tasks are handled within the system to ensure that no responsibilities slip through the cracks.
How VIZCare AI Powers VIZCare Empower
While Empower drives service execution and operational excellence, VIZCare AI delivers the intelligence layer that powers it, analyzing interaction context and orchestration signals in real time to guide precise, outcome-oriented actions
Example:
During a consumer interaction, VIZCare AI provides the right information, recommends next steps, and automates follow-ups, enabling faster resolution with minimal manual effort.
Leveraging orchestrated data and AI-driven guidance, VIZCare Empower can deliver consumer services that are accurate, error-free, and high-quality at scale.
Why the Suite Matters
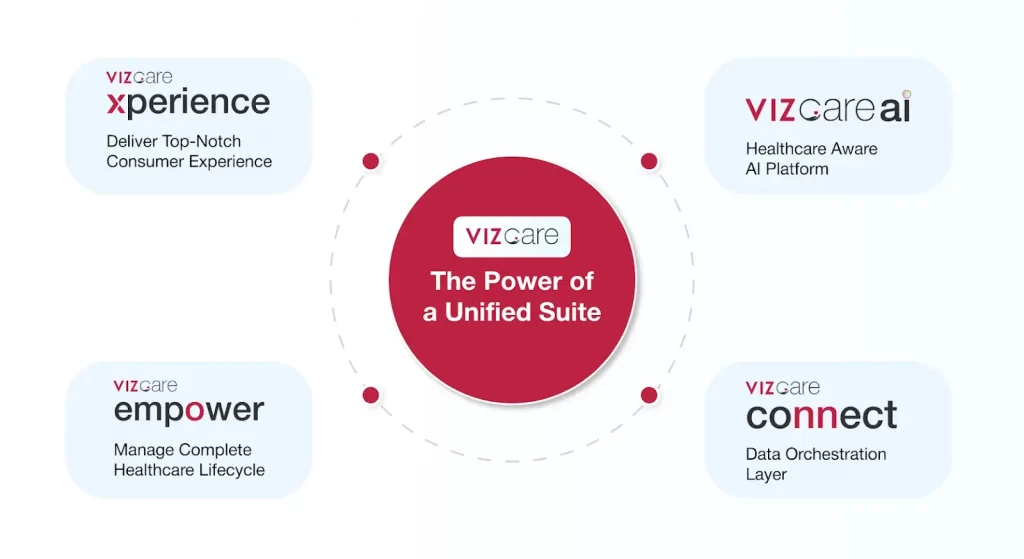
Individually, these platforms solve specific challenges. Together, they enable true intelligent orchestration:
- VIZCare AI serves as an intelligence layer
- VIZCare Connect ensures data is aligned
- VIZCare Xperience delivers seamless digital execution
- VIZCare Empower enables intelligent human intervention
This is how enterprise healthcare solutions move beyond automation to coordinated, adaptive, and scalable operations.

Why Enterprise Healthcare Needs to Move Beyond Automation Now
Enterprise healthcare operations are under mounting pressure. Regulations frequently alter, massive amounts of data keep growing fast, while interoperability demands keep rising forcefully. Within this sphere, traditional and static automated ways prove to offer no real miracles.
Key challenges that necessitate intelligent orchestration:
- Compliance Obligations: The healthcare field is almost in a litigious era over compliance. Automated systems are stationary and do not support rapid change, and have thus been found wanting in ensuring compliance with the latest legislative instruments.
- Interoperability Challenges: To communicate between various platforms, a healthcare system must easily utilize data. Existing tools struggle to provide the real-time data flow needed to make dynamic decisions.
- Data Explosion: The massive amount of data generated from member records and provider networks demands that systems be capable not only of automating but also of intelligently orchestrating so as to maintain accuracy and speed.
That is why getting past automation is already a current necessity and not a matter for the future. Intelligent orchestration acts as a link between business strategy and execution, thus helping organizations to remain flexible, compliant, and resistant to change at enterprise scale.

Wrapping Up
The evolution of the healthcare enterprise is clear:
- Past: Manual processing (High cost, slow, error-prone).
- Present: Task Automation (Slightly faster, but rigid and isolated).
- Future (2026+): Intelligent Orchestration (Adaptive, real-time, and scalable approach).
That entire transition from automation to orchestration to intelligence marks the definition of resilience for enterprise healthcare operations.
AVIZVA products: VIZCare Connect, AI, and Xperience together enable this transformation. Built for enterprise healthcare, it provides the orchestration foundation leaders need to improve operational efficiency, strengthen governance, and drive continuous improvement across the organization.
If your automation strategy is struggling at the last mile, it’s time to rethink the strategy. Contact AVIZVA and see how it enables intelligent orchestration at enterprise scale.

FAQs
- What’s the difference between healthcare automation and orchestration?
Healthcare automation refers to the process of performing separate tasks by using definite rules; for example, copying data or starting a workflow. Whereas orchestration connects and manages entire workflows across systems, adjusting in real time as data, rules, or conditions change.
- What use cases are best suited for intelligent orchestration?
Smart orchestration is most appropriate for multi-system processes with a constant need for coordination, for example:
- Real-time workflows that adjust instantly to eligibility, policy, or usage changes
- Proactive actions triggered by live risk or utilization signals
- Built-in compliance workflows with automatic governance and audit trails
- Cross-team coordination across operations, compliance, and engagement
- Adaptive prior authorization based on policy rules, thresholds, and SLAs
- How does orchestration integrate with existing EHRs and systems?
Modern service orchestration employs APIs, events, and standard interfaces to avoid replacing existing core systems. They act as a coordination layer that connects data and workflows across multiple existing platforms, enabling real-time synchronization with minimal impact on current investments.
- How to choose an orchestration platform for enterprise healthcare?
Health insurers need to seek out platforms that provide support for:
- Enterprise-wide workflow coordination
- AI-driven decision support
- Built-in compliance and auditability
- Easy integration with existing systems
A platform with the appropriate flexibility, transparency, and scalability will be more than merely automation.

