Table of Contents
Key Takeaways
1. Business Imperative: Healthcare provider engagement must keep pace with rising administrative
pressure, tighter timelines, and higher provider expectations.
2. The Problem: Traditional provider portals were built for status checks, not real work. They lack
context, slow critical workflows like prior authorization and credentialing, and drive rework, calls, and provider frustration.
3. The Shift: Provider engagement is evolving from static portals into intelligence hubs and connected environments that support real-time data, guided workflows, and in-platform collaboration.
4. The Solution: Platforms like VIZCare Xperience’s ProviderX bring insights and shared visibility into a single provider workspace.
5. Key Outcome: Faster resolution, fewer handoffs, improved provider trust, and measurable operational efficiency.
Provider portals were originally designed to reduce manual administrative requests, eliminate paperwork, and accelerate routine administrative workflows between payers and providers. For a significant period of time, they delivered on that promise. By 2026, however, many payer enterprises began to confront a different reality: portals that once improved efficiency were now introducing administrative friction, slowing high-stakes workflows, and contributing to growing provider dissatisfaction.
This shift is increasingly evident in the industry data. According to the American Medical Association, prior authorization alone remains a significant burden for providers: 94% report it delays access to needed care, and 95% say it contributes to burnout. When providers are unable to get timely, reliable answers within payer systems, the downstream impact is widespread across payer enterprises : increased call volume , more escalations, redundant rework, and strained provider network relationships.
It is this growing friction that is driving a change in healthcare provider engagement. What was once a static portal for claims status and document exchange is evolving into an intelligence-driven workspace that drives action and supports real workflows.
In this blog, we’ll explore why traditional provider portals are now a liability and what an intelligence hub looks like in practice. We’ll understand the key features to expect from a healthcare provider engagement platform in 2026, and what “good” looks like for payer teams planning the next phase of provider engagement.
Why Traditional Portals Are Now a Liability
A portal becomes a liability when it can no longer keep pace with the workflows it is meant to support. In 2026, provider workflows are increasingly time-sensitive, highly regulated, and heavily data-driven: far beyond the capabilities most traditional portals were designed to handle.
Costly Delays and Erosion of Trust
Traditional provider portals were originally designed to answer one narrow question: “What’s the status?” In today’s healthcare environment, that is no longer enough. Providers now require timely visibility across multiple critical areas, including prior authorization status and next steps, eligibility and benefit checks, reimbursement updates and remittance context, reconciliation questions such as payment exceptions and denials, and contracting or network updates.
Even when payers offer a portal, the process often remains slow. According to the 2024 CAQH Index, prior authorization continues to be one of the most time-consuming administrative tasks. Providers and staff spend an average of 16 minutes completing a prior authorization via a health plan portal and 24 minutes when using phone, fax, or email. When these minutes are multiplied across thousands of authorizations and multiple lines of business, they quickly add up, creating a substantial administrative burden that drives costly delays and erodes provider trust.
Lack of Context-Aware Experience Across Provider Interactions
Many traditional portals treat each provider interaction as a standalone event. Providers submit a question, upload a document, or check a status, only to start over again the next day. These systems fail to carry context across tasks, leaving critical information disconnected.
For example, a portal often does not link a prior authorization request to its clinical attachment, a claim denial to the corresponding contract term, a credentialing step to a missing document, or a provider’s network status to payment timing. As a result, providers must repeatedly re-enter information, navigate complex menus, and explain the same issue to multiple teams – adding frustration, inefficiency, and administrative burden.
Network Onboarding and Credentialing Bottlenecks
Credentialing and network onboarding remain slow and opaque in many payer enterprises. Even when a payer provides a portal, the onboarding process often depends on email threads, manual checklists, disconnected document storage, unclear ownership across teams, and limited visibility for providers. This is where the traditional portal model breaks down.
Provider onboarding is not a single form submission; it is a complex, multi-step workflow that requires role-based routing, real-time status transparency, automated document validation, and clarity on next steps. Without these portal capabilities, providers experience delays, repeated follow-ups, and frustration, while payers face inefficiencies and increased administrative burden.
The Shift Toward Provider Engagement Intelligence Hubs
A traditional portal answers questions; an intelligence hub prevents them from arising in the first place.
This is the fundamental shift in healthcare provider engagement in 2026. Payer organizations are moving beyond the ‘log in and check status’ model toward a connected, intelligence-driven workspace where providers can complete tasks efficiently, access context-rich information, and navigate workflows seamlessly: forming the foundation of next-generation provider engagement solutions.
This evolution signals a broader transformation in how provider engagement solutions for payers are designed, measured, and optimized.
What is an intelligence hub?
In today’s complex healthcare ecosystem, providers often navigate multiple systems to manage authorizations, claims, credentialing, and payments. An intelligence hub changes that by offering a single, integrated workspace that streamlines operations and enhances collaboration.
Key capabilities of an intelligence hub include:
- Real-time operational updates across authorizations, claims, credentialing, contracting, and payments.
- Guided workflows and next-best-action recommendations.
- Integrated communication for seamless collaboration with payer teams.
- Advanced analytics that surface trends, risks, and delays.
- Future-proof automation that eliminates manual routing and repetitive tasks.
By consolidating all tools and insights into one platform, an intelligence hub shifts providers from managing multiple portals to working in a centralized workspace. Platforms like VIZCare ProviderX enable providers to initiate and track queries, upload and retrieve documents, and access analytics, all without leaving the hub.
The result is an efficient and transparent experience for providers, coupled with enhanced operational visibility and a lighter administrative burden for payers..
How Intelligence Hubs Surface the Right Information at the Right Time
The ‘intelligence’ in an intelligence hub goes beyond simply leveraging AI – it reflects the platform’s ability to deliver the right information at the right time. A well-designed intelligence hub ensures providers receive timely, actionable updates, reducing delays and making engagement more efficient and seamless.
Some examples of these updates include:
- Authorization updates and missing items
- Credentialing progress, holds, and document gaps
- Contracting milestones and next steps
- Payment exceptions and reconciliation context
By surfacing information precisely when it’s needed, intelligence hubs minimize portal search time, one of the most common hidden costs in provider engagement. This creates a more efficient, transparent, and seamless experience for both providers and payers.
How Intelligence Hubs Enable Integrated Communication
In traditional provider portals, communication often happens outside the workflow, across multiple channels such as phone, email, fax, ticketing systems, and scattered internal tools
Intelligence hubs embed communication directly into the workflow, ensuring all conversations and exchanges are contextual and traceable.
Some examples of this integrated communication include:
- Threaded conversations are tied to specific requests for clarity and continuity.
- Internal notes for payer teams to collaborate efficiently.
- Document sharing with version control for accurate record-keeping.
- Audit trails to support compliance and dispute resolution.
By integrating communication into the workflow, intelligence hubs help payers and providers stay aligned, reduce back-and-forth, and eliminate unnecessary administrative overhead.
Key Features of Modern Provider Engagement Platforms
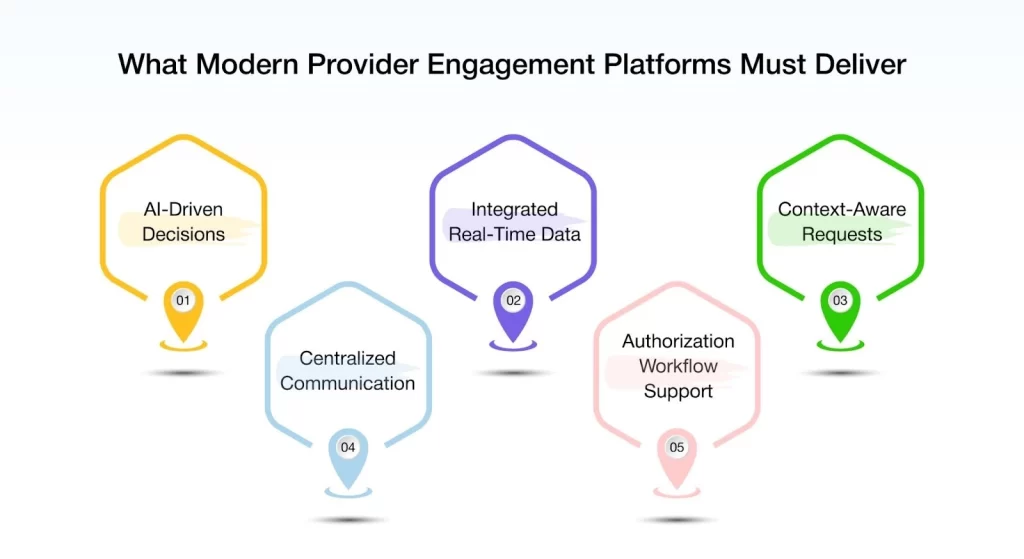
Choosing the right provider engagement software for healthcare organizations starts with capabilities that teams will actually use.
In 2026, a modern provider engagement platform is defined by capabilities that not only streamline payer operations but also strengthen provider relationships and drive overall network performance.
The following are some of the key features every modern provider engagement platform should include:
1. AI-Powered Decision-Making
AI becomes truly practical in provider engagement when it speeds up work instead of adding complexity. In a modern provider engagement platform, AI supports teams in the following ways:
- Intelligently triage and route requests to the right team, the first time.
- Summarize requests and attachments to save manual review time.
- Recommend next steps based on plan rules and historical patterns.
- Detect missing information before submission to reduce rework.
- Identify repeat issues to prevent recurring workload.
The result is fewer handoffs, less back-and-forth, and faster resolution, allowing teams to focus on higher-value work.
2. Real-Time Data Sharing and Integrated Analytics
Traditional provider portals often lag behind real-time operations, leaving both providers and healthcare teams frustrated. Status updates arrive too late, explanations for delays are unclear, and analytics remain siloed, disconnected from the workflow.
In 2026, these gaps are increasingly unacceptable, especially as CMS drives the industry toward faster, more transparent prior authorization processes. A modern provider engagement platform addresses these challenges by providing :
- Real-time status updates with clear decision context, keeping providers informed and reducing unnecessary follow-up.
- Integrated analytics that track workload, cycle times, and bottlenecks in a single, unified view.
- Cross-workflow visibility, offering insights across processes rather than within isolated modules.
The result is faster, more transparent operations, reduced manual work, and stronger alignment between payers and providers.
3. Intelligent Request Management
Next-generation provider engagement platforms manage requests intelligently, ensuring they reach the right team at the right time. Rather than routing everything to a generic queue, modern provider engagement platforms perform the following functions:
- Automatically direct requests to the appropriate team based on type and complexity.
- Prioritize requests according to urgency and impact.
- Provide clear status updates and guided next steps for providers.
The result is reduced back-and-forth communication, faster resolution, and greater provider confidence that their requests are being handled efficiently.
4. Centralized Communication
Providers and payer teams need a shared record of truth to stay aligned and work efficiently. Modern provider engagement platforms centralize communication by offering:
- Direct in-platform messaging tied to each case for context-rich conversations.
- Shared notes and internal collaboration to keep teams coordinated.
- Document exchange with version control to ensure accuracy and traceability.
- Audit trails to support compliance and dispute resolution.
This capability is critical because communication gaps are a major driver of frustration and distrust. When providers cannot see what’s happening, they often assume nothing is being done. A unified collaboration layer ensures transparency, accountability, and confidence in the process.
5. Workflow-Ready Prior Authorization Support
Prior authorization remains a core workflow affecting provider experience. Modern provider engagement platforms streamline this process in the following ways:
- Providing real-time authorization status and clear next steps for providers.
- Minimizing manual resubmissions and reducing administrative burden.
- Attaching clinical documentation automatically to the correct request context.
- Reducing time spent chasing updates across multiple channels.
The result is faster prior authorization workflows, fewer errors, and improved provider satisfaction. CAQH underscores the scale of administrative burden across provider-plan interactions. According to a CAQH report, the healthcare industry spends $83 billion annually on staff time for routine administrative transactions between providers and health plans, with providers shouldering the majority of that cost.
This is precisely why intelligent provider engagement hubs are essential: they reduce administrative waste where it matters most, freeing teams to focus on higher-value work and improving overall efficiency.
How VIZCare Xperience Powers the Shift to Provider Engagement Intelligence Hubs
The shift from traditional provider portals to intelligence hubs in healthcare is real. Top healthcare enterprises now view provider engagement as a connected, intelligent operating layer and not just a static interface.
VIZCare ProviderX is purpose-built to power this transformation. It is an AI-powered, feature-rich platform that equips providers with the tools, insights, and transparency they need to deliver quality care with confidence.
1. Intelligent AI-Driven Assistance and Insights
ProviderX embeds AI directly into provider workflows to reduce back-and-forth, anticipate issues, and accelerate resolution:
- AI-assisted prior authorizations with likelihood prediction.
- Contextual clinical insights delivered at the point of interaction.
- Smart denial identification with appeal guidance.
- Proactive nudges for pending actions and documentation
2. Seamless Pre-Service Engagement
Most provider engagement friction occurs before care is delivered. ProviderX provides real-time visibility and actionable guidance to ensure providers are prepared operationally and financially:
- Real-time eligibility and benefits verification.
- Digital prior authorization submission and tracking.
- Upfront price and reimbursement estimates.
- Readiness checks to prevent missing or incomplete data
3. Proactive Post-Service Coordination
After care delivery, providers need structured, efficient ways to complete documentation and coordinate next steps without emails, portal hopping, or lost context. ProviderX streamlines post-service workflows in the following ways:
- Secure service documentation uploads.
- Shared care coordination across providers.
- Direct member communication within the platform.
- Guided claim submissions with validation checks
4. Transparent Post-Adjudication Support
After claims submission, providers need clarity, visibility, and actionable next steps. ProviderX keeps engagement active throughout adjudication in the following ways:
- Real-time claim status updates with clear progress indicators.
- ERA access for faster reconciliation.
- Guided denial explanations and appeal workflows.
- Audit-ready histories for compliance and reporting.
5. Streamlined Provider Onboarding & Network Management
ProviderX replaces slow, paper-heavy onboarding with guided, digital-first workflows that simplify provider management:
- Self-service provider onboarding and registration.
- Digital credentialing with automated alerts and renewals.
- Contract lifecycle tracking with real-time status visibility.
- Real-time network insights across specialties and regions.
- Hassle-free provider profile updates.
Provider Engagement Doesn’t Evolve in Isolation
The shift from traditional portals to intelligence hubs extends beyond individual providers. Healthcare engagement platforms deliver maximum impact when they function as part of a connected ecosystem, where every stakeholder operates from shared context, real-time data, and coordinated workflows.
VIZCare Xperience is built to make this transformation seamless. VIZCare Xperience is a comprehensive suite of AI-enabled web portals and native mobile applications designed to address the unique needs of every stakeholder across the healthcare insurance ecosystem.
- MemberX: The portal is a one-stop shop for members to manage their coverage, search for benefits, find care, understand claims, and track prior authorizations. While it primarily focuses on enabling ease of self-service, thereby reducing operational workload for enterprises, it also simplifies and enhances interactions with member engagement teams.
- BrokerX: The portal is designed to simplify client acquisition, management & retention for agencies & agents. It brings capabilities to manage the entire lifecycle of clients, covering pre-sales, sales, and post-sales at fingertips. Some of the most-used and high-impact features include quoting and proposals, managing their book of business, accessing commission statements, and having ready access to insightful analytics.
- EmployerX: With employers’ needs in mind, the portal is designed to enable effortless management and oversight of employee benefits and usage. Employers can easily manage their group membership, including open enrollment, life change events, member profile information, understanding plan benefits, invoices, and plan performance.

The Road to the Future: What’s Next for Provider Engagement?
As broader healthcare provider engagement trends 2026 reshape the industry, collaboration frameworks between payers and providers will continue to evolve.
Rising administrative burden, ongoing workforce constraints, growing expectations for faster access, stricter compliance requirements, and the increasing need for real-time, shared data are all pushing healthcare organizations to rethink how engagement is designed and delivered.
Key trends shaping the future include:
- AI-driven personalization that adapts to provider behavior and preferences.
- Predictive analytics that anticipate provider needs and workflow spikes.
- Automation that continuously optimizes processes as regulations and policies evolve.
How To Start Planning Now?
If your organization still views the provider portal as just ‘a channel,’ it’s time to reframe it as ‘an operating system’ for provider work. Here are the steps to get started:
- Map high-volume, high-friction provider workflows.
- Identify points where context is lost: handoffs, email threads, duplicate requests.
- Define key ‘hub’ outcomes: request cycle time, first-touch resolution, repeat follow-ups.
- Choose a platform designed for workflows, not just a portal UI.
- Roll out in phases, starting with the highest-friction workflows
For organizations aiming to adopt the best practices in provider engagement for value-based care in 2026, this shift is critical. Value-based models require faster alignment, clearer communication, and shared visibility across care and payment workflows.
Final Thoughts
In 2026, provider engagement is no longer just about offering a portal to the providers.
It’s about creating a working environment that reduces friction, preserves context, and helps both providers and healthcare insurance teams complete tasks faster – with fewer calls, emails, and repeated submissions.
If your organization is planning the next phase of healthcare provider engagement, you need to ask yourself: Is your platform just for checking status, or for actually getting work done?
Schedule a call to see how VIZCare ProviderX transforms provider engagement.

FAQs
1. What is healthcare provider engagement, and why is it important?
Healthcare provider engagement refers to how payers use intelligent portals to give providers real-time visibility, guided workflows, and collaborative tools across pre-service, post-service, and network management activities. Moreover, strong provider engagement reduces friction across authorizations, claims, onboarding, and payments—directly impacting cost control, turnaround times, and network satisfaction.
2. What features should a provider engagement platform include?
A modern platform should support:
- Real-time status visibility across workflows
- Context-aware, guided request handling
- Integrated communication and document exchange
- Analytics and AI to reduce rework and delays
These features help payers move from reactive servicing to proactive ope
3. How do portals evolve into intelligence hubs for provider engagement?
Portals evolve into intelligence hubs when they shift from static access points to workflow-driven environments. This includes embedding real-time data, transparency, analytics, and in-platform collaboration to ensure work progresses without repeated follow-ups or context loss.
4. What are the common barriers to successful provider engagement?
Common barriers include:
- Static portals with limited workflow support
- Disconnected systems and delayed updates
- Manual routing and unclear ownership
- Communication happens outside the platform
These gaps increase administrative effort and slow resolution.
5. How will provider engagement platforms evolve in 2026 and beyond?
In 2026 and beyond, provider engagement platforms will rely on AI to deliver smarter, more connected engagement across areas like:
- Routing, prioritization, and guidance
- Predictive analytics for forecasting volume and problems
- Being part of the combined engagement ecosystem
The focus will be redirected from being the one liable for basic accessibility to the one responsible for final results and large-scale efficiency.

