Table of Contents
Key Takeaways
- Interoperability is still a major payer challenge.
- Legacy systems create data delays and silos.
- Poor data flow affects claims, authorizations, and member experience.
- Real progress needs standards, APIs, HIEs, and cloud systems.
- Better interoperability improves efficiency, compliance, and decision-making.
- AVIZVA’s VIZCare Connect helps solve these gaps at scale.
Healthcare interoperability remains a persistent challenge, not due to missing standards across healthcare systems but because many organizations continue to approach it as a compliance requirement rather than a strategic business priority.
Many payer organizations are still operating on outdated, fragmented systems or point solutions that struggle to integrate effectively. Over time, these silos lead to delayed data flow, increased reliance on manual workarounds, and slower decision-making. When systems cannot seamlessly exchange information, it results in longer claims processing times, delayed authorizations, and ultimately a compromised consumer experience.
Understanding healthcare system integration challenges begins with recognizing how deeply these operational gaps affect every layer of a payer organization. With regulations such as CMS-0057-F coming into effect in 2026, the pressure to close these gaps is growing.
At AVIZVA, we believe interoperability should be embedded into everyday operations, not layered on later to meet compliance requirements. Systems should work together to enable secure, accurate, and real-time data exchange, driving efficiency, faster decisions, and improved member outcomes.
In this blog, we explore the key interoperability & healthcare system integration challenges payers face today and outline a practical, scalable approach to addressing them with AVIZVA’s future-proof solutions.
The Payer’s Dilemma in 2026: Critical Challenges in Healthcare Interoperability
Most payer organizations rely on multiple point solutions to manage different parts of the insurance lifecycle, such as claims platforms, eligibility and enrollment systems, price transparency tools, provider network databases, care management tools, broker and employer portals, and regulatory reporting systems. Over time, these systems have been added incrementally. While they may be technically connected, they rarely function together in real time.
As a result, data inconsistencies and delays are common. Claims data may not align with eligibility records, provider information may vary across systems, and authorizations can be delayed due to missing or incomplete data. Member and broker portals often reflect outdated information, further impacting experience and trust.
Interoperability, in simple terms, means enabling these systems to exchange accurate data instantly and securely, without the need for manual intervention.
For payers in 2026, healthcare system integration challenges are no longer just an IT concern; they are at the core of how effectively data flows across claims systems, provider networks, partner platforms, and regulatory systems to enable faster decisions and more efficient service delivery.
Key Healthcare Interoperability Challenges
1. Incompatible Systems
Many healthcare organizations continue to rely on legacy and disconnected systems that do not integrate effectively. These silos hinder cross-functional communication, limit real-time data sharing, and create inefficiencies across operations.
2. Inconsistent Data
Payers struggle with inconsistent and poorly standardized data across systems. Variations in formats, definitions, and terminology create semantic gaps that hinder accurate interpretation, limit seamless data exchange, and impact overall decision-making.
3. Security Risks
Payers must ensure that sensitive healthcare data is secure and compliant across all systems. Laws such as HIPAA, PHI or GDPR require strict adherence, and violations can result in significant fines and loss of trust among members and regulators. At scale, the challenge is less about encryption and more about managing access, maintaining visibility, and ensuring accountability across interconnected systems.
4. Governance Gaps
Many payer organizations struggle to manage who can access which data across functions and external partners. Legacy systems often lack a ‘secure-by-design’ framework, making it difficult to enforce proper controls, maintain accountability, and ensure compliant data use across the enterprise.
5. Cost Burden And Resource Strain
Payer organizations face significant financial and resource demands when implementing and maintaining interoperability solutions. While much of the focus remains on the cost of compliance, the larger and often overlooked burden comes from ongoing operational inefficiencies – where teams rely on manual workarounds to bridge gaps between systems, driving up costs and limiting scalability.
6. Scalability Constraints
Many interoperability setups struggle to support real-time use cases and evolving digital initiatives, limiting organizational agility. Adding new partners often requires extensive custom coding and long implementation cycles, making it difficult for organizations to scale quickly and respond to changing member demands.
The Real Impact on Payers
When these interoperability challenges persist, their impact is felt across the entire organization. Claims and authorization workflows slow down, administrative overhead rises, and compliance risks increase. At the same time, members, providers, brokers, and employers often experience inconsistency in their interactions.
Thus, interoperability gaps don’t remain confined to IT; they directly affect operational efficiency and the reliability with which payers serve their broader ecosystem.
How to Address Healthcare Interoperability Challenges: A Strategic Approach
Solving healthcare interoperability challenges requires more than simply adding more integrations; it calls for a shift in mindset. What’s truly needed is a well-designed, scalable, and continuously maintained data ecosystem that allows information to flow securely, consistently, and in real time.
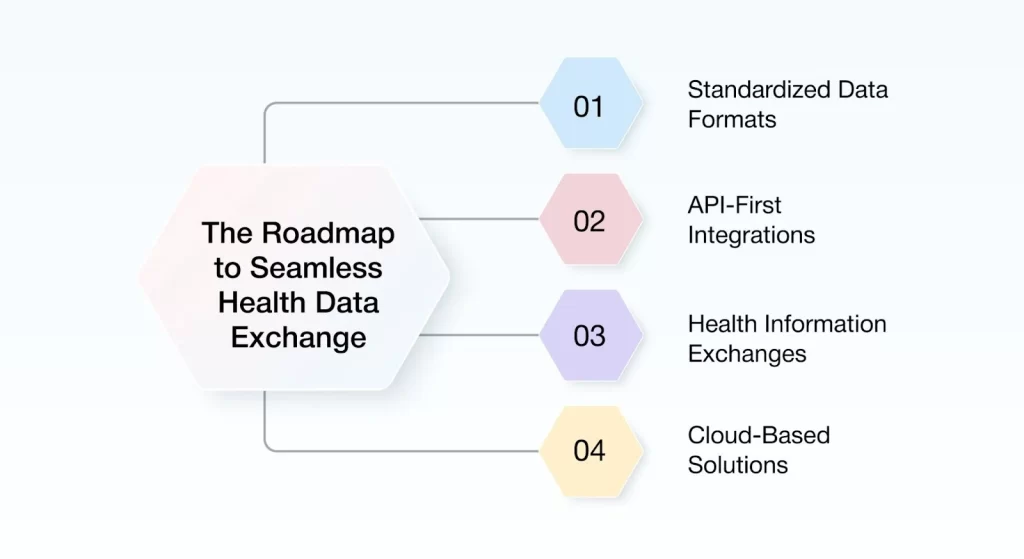
The following strategic building blocks lay the foundation for sustainable healthcare data solutions.
1. Standardized Data Formats
Highly structured and universally understandable healthcare data is achieved through widely recognized standards such as FHIR (Fast Healthcare Interoperability Resources), HL7, and CDA. These standards serve as the backbone of effective interoperability, enabling seamless data exchange between disparate systems.
By adopting these standards, healthcare organizations can ensure that all systems speak the same language, improving data consistency and supporting more reliable, real-time workflows.
2. API-First Integrations
APIs (Application Programming Interfaces) are a key enabler for bridging gaps between disparate systems. By adopting an API-first approach, healthcare organizations can build scalable, real-time integrations across multiple platforms, ensuring that critical data is always available when and where it’s needed.
Organizations moving toward API-first strategies are experiencing improved interoperability, enhanced decision-making capabilities, and more efficient workflows through automation, creating a more connected and responsive healthcare ecosystem.
3. Health Information Exchanges
Health Information Exchanges (HIEs) play a critical role in enabling seamless data exchange between insurers, providers, and other healthcare stakeholders. By connecting to EHRs, health systems, and national networks, HIEs provide accurate, real-time information at the point of care while adhering to federal and state privacy regulations, including HIPAA.
The key to maximizing their value is ensuring that HIE data integrates smoothly into payer workflows, rather than becoming another disconnected source, thereby supporting efficient, timely, and informed decision-making.
4. Cloud-Based Solutions
Cloud platforms offer the scalability and resilience needed for secure, real-time & secure healthcare data exchange. By leveraging cloud-based solutions, healthcare organizations can ensure that data is always available when needed. They can further centralize security and monitoring, improve cross-team collaboration, and accelerate the deployment of new interoperability capabilities.
Cloud-based approaches also support future growth, enabling organizations to scale without adding strain to core systems, creating a more agile and connected healthcare ecosystem.
By leveraging modern APIs, FHIR-compliant standards, and cloud technologies, AVIZVA delivers a seamless and scalable solution for healthcare organizations, enabling secure, consistent, and real-time data interoperability.
Key Healthcare Interoperability Benefits
Once healthcare organizations overcome interoperability challenges, the true value of seamless data exchange begins to emerge. The benefits become clear across operations, decision-making, and overall business performance. Let’s take a closer look :
1. Improved Outcomes For All Stakeholders
Seamless data exchange ensures that accurate, up-to-date information is available to all stakeholders – exactly when and where it’s needed.
- Internal Teams: A unified, real-time view of claims, eligibility, and services reduces manual reconciliation, accelerates decision-making, and enables more proactive issue resolution.
- Providers: Timely access to eligibility, authorizations, and claims status minimizes back-and-forth communication, reduces delays, and supports faster, more confident care delivery.
- Members: Consistent data across touchpoints improves clarity around coverage and claims, shortens resolution times, and builds trust by reducing unexpected outcomes.
- Brokers And Employers : Real-time visibility into enrollments, billing, and plan performance enables smoother renewals, stronger reporting, and better alignment across stakeholders.
- Increased Operational Efficiency
When systems are unified, operational efficiency improves significantly. Organizations benefit from faster claims adjudication and authorizations, reduced data redundancy across systems and teams, and more streamlined workflows with fewer handoffs.
2. Stronger Regulatory Compliance
Seamless interoperability helps healthcare organizations meet regulatory requirements while maintaining high standards of data security and privacy. By enabling consistent, traceable data exchange, organizations can better align with regulations such as HIPAA and reduce compliance risks.
Adopting FHIR standards and secure APIs further strengthens this foundation, helping insurers avoid costly penalties while maintaining the trust of their members.
3. Agility For Future Growth
Interoperable systems provide the flexibility needed to support new technologies, and partnerships. With a scalable interoperability foundation, healthcare organizations can integrate new platforms and solutions more quickly, support advanced analytics and AI initiatives, and adapt to regulatory and market changes with minimal disruption.
This level of agility positions organizations for sustained, long-term growth rather than short-term fixes.
Why AVIZVA is the Right Partner for Solving Interoperability Challenges
In healthcare payer organizations, communication between systems often breaks down long before data reaches its intended destination. Claims, eligibility, provider networks, clearinghouses, and regulatory systems rarely operate in sync. Instead, they function in parallel, using different formats, protocols, and timelines, which makes achieving true interoperability a persistent challenge.
When interoperability is treated as an afterthought, these disconnected pathways create delays, inconsistencies, and increased risk. To overcome today’s healthcare interoperability challenges, data exchange must be built into the foundation – engineered for seamless integration – rather than patched together through temporary fixes.
This is where AVIZVA’s VIZCare Connect plays a critical role. It is a healthcare data connectivity platform designed to address the end-to-end data integration and interoperability needs of healthcare enterprises.
Engineered for scale, it orchestrates millions of transactions across disparate systems while preserving data accuracy and lineage.
| Interoperability Challenge | The VIZCare Connect Benefit |
| Disconnected claims, eligibility, and provider data | Unifies data exchange through a centralized interoperability layer |
| Point-to-point integrations | Enables reusable, scalable orchestration across systems and partners |
| Varied data formats and semantics | Standardizes and validates data using rules-driven transformation |
| Manual data handling slows workflows | Automates routing, enrichment, and validation end-to-end |
| Limited data flow visibility | Provides real-time insight into data movement and bottlenecks |
Key Capabilities Of VIZCare Connect
1. Real-Time Data Orchestration & Synchronization
The platform supports a wide range of integration protocols and formats, automates complex data flows, and leverages built-in AI to dynamically configure sources, map fields, and optimize transformations.
2. A Robust Suite Of 300+ Healthcare APIs
The platform offers a suite of healthcare APIs to accelerate internal product development and unlock enterprise-grade innovation at scale. The healthcare APIs are purpose-built to support lookup, read, search, add, and update functions across all key healthcare data types.
3. Preloaded & Continuously Updated Healthcare Industry Data
The platform provides an enriched, ready-to-use dataset that complements enterprise data, enabling enhanced analytics, decision-making, and AI-driven insights.
4. 360° Data Views For Business & Operational Intelligence
The platform delivers end-to-end visibility across all systems and touch points, providing real-time insights and analytics to drive scalable, accurate, and efficient healthcare operations.

Conclusion
The path to overcoming healthcare interoperability challenges is clear: shift from viewing data exchange as a burden to seeing it as a driver of growth. By leveraging standardized data formats, API-first integrations, and real-time orchestration, your healthcare organization can achieve member-centricity and regulatory compliance while maintaining operational efficiency.
AVIZVA helps healthcare organizations address interoperability challenges with a practical, proven, and scalable approach. Through VIZCare Connect, AVIZVA enables enterprises to drive end-to-end healthcare data connectivity with unmatched visibility and transparency.
Want to explore more about VIZCare Connect? Book a demo now.
FAQs
1. What are the major healthcare interoperability challenges payers face today?
Healthcare payers face several challenges in achieving seamless data exchange:
- Technical fragmentation: Multiple disconnected systems make it difficult to integrate data across various platforms.
- Data quality and semantic gaps: Inconsistent data formats and terminologies lead to errors in managing claims and other critical data.
- Privacy and compliance risks: Ensuring secure, compliant data sharing is challenging, especially with complex regulatory requirements.
2. What role do data security and privacy play in interoperability challenges?
Data security and privacy are critical to ensuring compliance and building trust:
- HIPAA compliance: Healthcare payers must ensure that all data exchanges adhere to strict privacy regulations.
- Data breaches: Failure to maintain robust security can lead to costly breaches and reputational damage.
- Secure data sharing: Balancing accessibility with security is essential to ensure data integrity and protect member information.
3. What steps can healthcare providers take to overcome interoperability challenges?
Healthcare payers can take several steps to improve interoperability:
- Adopt standardized data formats, such as FHIR, to improve data consistency.
- Leverage API integrations to ensure seamless, real-time data exchange across systems.
- Utilize cloud-based solutions to enhance scalability, security, and data sharing capabilities.
- Implement data governance frameworks to ensure compliance and accurate data exchange.
4. Are regulations helping or complicating healthcare interoperability challenges?
Regulations can be instrumental in providing a sense of direction and urgency; however, they can also reveal shortcomings of the existing systems. Even though the mandates are accelerating the need for data sharing, many payers are finding it difficult to implement compliance at scale.
Companies that have a standardized, well-controlled interoperability framework are more capable of efficiently adapting to regulatory requirements without experiencing additional complexity.

