Table of Contents
| TL;DR Business Imperative: Deliver faster, clearer, and more human insurance conversations at scale. Problem: Chatbots and scripted journeys break when real insurance questions get complex. Solution: Use insurance-ready conversational AI, like AVIZVA’s VIZCare AI, that understands intent, remembers context, and takes action in real-time. Key Outcome: Less friction, fewer handoffs, and insurance experiences members actually trust. |
Healthcare insurance interactions are becoming more frequent, more complex, and significantly more time-sensitive. Legacy engagement models like static scripts, IVRs, and basic chatbots were designed for a simpler era. In 2026, they will no longer be sufficient to meet rising member expectations or operational demands.
This is where conversational AI in healthcare insurance is fundamentally redefining engagement.
Modern conversational AI platforms are no longer limited to deflecting basic FAQs. They now support multi-step, real-time workflows across multiple use cases such as eligibility checks, coverage and benefits explanations, claims guidance, proposal and quotes generation, onboarding & enrollments, and compliance-driven communications delivered with accuracy, context, and continuity.
As insurers prepare for 2026, the shift is clear:
- Reactive support → Always-on, proactive engagement
- Static scripts → Intent-driven, adaptive conversations
- Channel-specific interactions → Continuous, context-aware journeys
This evolution has moved conversational AI healthcare solutions from experimental pilots to business-critical infrastructure that are central to both member experience and operational efficiency.
In this blog, we explore how conversational AI is reshaping healthcare insurance services, examine real-world use cases and business impact, and highlight how AVIZVA’s VIZCare AI enables secure, compliant, and scalable conversations that meet the demands of modern healthcare ecosystems.
Why Insurance Needs More Than Chatbots in 2026
Early chatbots were built for simple deflection like answering FAQs, routing requests, or reducing call volumes. They were never designed for the complexity of healthcare insurance. As consumer interactions now span eligibility, coverage interpretation, billing inquiries, and compliance-sensitive scenarios, static bots fail when context, judgment, or real-time system access is required.
In 2026, insurers don’t need more chatbots. They need conversational intelligence capabilities that can understand intent, access live data, and guide interactions end-to-end across the member journey.
What Has Changed Since the First Chatbot Wave
Modern conversational AI is fundamentally different from its predecessors. The shift is not incremental, it is architectural:
- Intent understanding beyond keywords, powered by large language models(LLMs) that interpret nuance, not just commands
- Live access to core insurance systems, enabling real-time, accurate responses rather than scripted replies
- Dynamic, rule-aware answers, grounded in policy logic, benefit configurations, and compliance requirements
- Seamless escalation to human teams, with full conversational context preserved
This evolution moves AI from answering isolated questions to resolving underlying intent, a critical distinction for insurance interactions.
What “Conversational AI” Actually Means Today
What truly differentiates modern conversational AI is the intelligence layer behind it that simplifies insurance complexity in real-time. In 2026, conversational AI is about delivering experiences that are seamless, efficient, and genuinely member-centric.
Key Capabilities include :
- Context awareness across multi-turn interactions
The system understands what has already been discussed and why the member is reaching out eliminating repetition and confusion. - Memory across conversations and channels
Interactions don’t reset when a member switches from web to mobile, or returns days later. Context persists across time and channels. - Real-time orchestration across systems
Claims, policy, billing, and eligibility workflows are coordinated behind the scenes, so consumers receive answers, not transfers. - Human–AI collaboration
AI handles structured, repeatable tasks at scale, while human agents step in for judgment-intensive, sensitive, or exception-driven scenarios.
Together, these capabilities make conversational AI suitable for decision-grade interactions, not just self-service deflection.
Why This Shift Is No Longer Optional
Several forces are converging to make conversational AI a necessity, not a differentiator for insurers:
- Interaction volume has outpaced human capacity
Service demand continues to grow, but scaling teams linearly is no longer viable. - Policy and regulatory complexity keep increasing
Consumers need clearer explanations, not more documents or transfers. - Speed has become a trust signal
Delayed answers erode confidence, even when the final response is correct. - Data exists, but is locked behind systems
Conversational AI unlocks that data and delivers it in a usable, human format.
In 2026, the question is no longer whether insurers should adopt conversational AI, but whether they are deploying it with the intelligence, integration, and governance required to truly transform member experience.
| Takeaway: Members don’t experience insurance in workflows—they experience it in conversations. |
Real-World Conversational AI Use Cases That Actually Matter in 2026
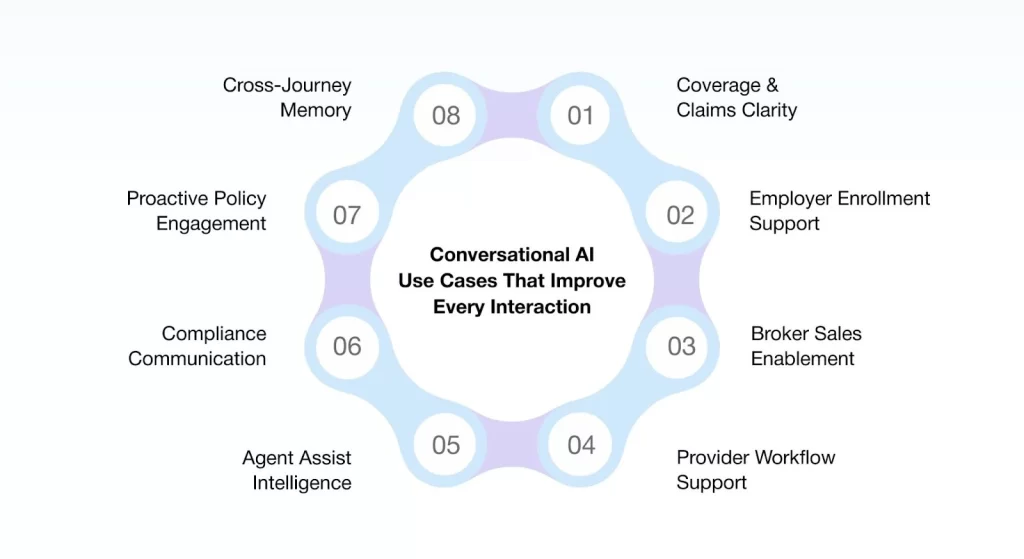
Conversational AI matters only if it makes insurance experiences better, and not more complex. The following conversational AI use cases in healthcare insurance demonstrate how insurers are simplifying complexity, reducing friction, and aligning with stakeholders’ intent throughout the service lifecycle.
- Member Experience: Coverage, Claims & Clarity at the Moment of Need
Coverage and claims conversations are often complex and emotionally charged. Conversational AI simplifies these interactions by delivering:
- Plain-language explanations of benefits and exclusions
- Context-aware answers tied to a member’s specific policy
- Follow-up clarification without restarting the conversation
Example:
A member asks, “Is this MRI covered?”
Instead of a scripted FAQ reply, conversational AI checks their plan, explains coverage limits, mentions prior authorization if needed, and clarifies expected out-of-pocket costs, all in one single conversation.
- Employer Support: Enrollment, Billing & Workforce Updates Without Tickets
Employers managing group plans deal with recurring operational tasks: enrollment changes, invoice queries, employee additions, and policy clarifications. Conversational AI enables:
- Guided employee enrollment management
- Real-time invoice and payment clarification
- Eligibility updates without manual form entries
- Renewal and compliance reminders
Example:
An HR administrator asks, “An employee got married. So now how do I add their spouse to our group health plan?”
The AI validates the qualifying life event window, confirms required documentation, updates dependent coverage in the core enrollment system, adjusts premium contributions, and generates a confirmation record for payroll reconciliation.
- Broker Enablement: Quotes, Plan Comparisons & Commission Visibility
Brokers operate in high-speed environments where responsiveness affects revenue. Conversational AI supports brokers with:
- Instant quote generation
- Plan comparison guidance
- Commission tracking insights
- Onboarding status updates
Example:
A broker asks, “Compare these two plans for a 50-employee group.”
The AI highlights premium differences, benefit variations, employer contribution impact, and underwriting considerations, enabling faster decision-making.
- Provider Support: Eligibility, Prior Authorizations & Claims Guidance
Providers need fast answers to administrative questions that affect member care timelines. Conversational AI assists with:
- Real-time eligibility verification
- Prior authorization requirements
- Claim submission guidance
- Payment clarification
Example:
A provider asks, “Does this customer require prior authorization for this procedure?”
The AI checks plan rules, confirms requirements, explains documentation needed, and guides next steps, reducing back-and-forth calls.
- Contact Center & Operations: Assisted Intelligence for Live Agents
Conversational AI is not just customer-facing. It also strengthens internal operations by supporting agents during live interactions. It enables:
- Real-time intent detection during calls
- Suggested next-best responses
- Auto-generated call summaries
- Automated post-call workflows
Example:
During a call about a denied claim, the AI identifies the denial reason, surfaces the relevant benefit rule, checks appeal timelines, and prepares a compliant explanation script for the agent, while automatically generating structured case notes.
- Compliance & Regulatory Communication Across Stakeholders
Healthcare insurance communication must be accurate, timely, and auditable. Conversational AI supports:
- Policy change notifications
- Regulatory disclosures
- Acknowledgment tracking
- Rule-based response validation
Example:
A regulatory update changes telehealth coverage rules.
The AI proactively notifies affected employer groups and members, explains the impact based on plan configuration, confirms acknowledgment, and logs the interaction for compliance reporting.
- Proactive Engagement Across the Policy Lifecycle
Instead of reactive servicing, conversational AI enables contextual, event-driven outreach for all stakeholders. This includes:
- Renewal reminders tailored to usage patterns
- Missing documentation nudges
- Enrollment completion prompts
- Broker follow-up reminders
Example:
During open enrollment, a member asks, “If I keep my current plan, will my doctor still be covered next year?”
The AI checks whether the doctor is still part of the plan’s network, confirms what the member would pay for visits, explains if any rules have changed, and shows nearby covered doctors if needed. This helps the member choose a plan with confidence before submitting enrollment.
- Cross-Journey Memory That Eliminates Re-Explanation
Insurance conversations don’t happen in a single session. Stakeholders switch channels, pause processes, and return later. Conversational AI delivers:
- Persistent context across web, mobile, and assisted channels
- Continuity between digital and live interactions
- Fewer repeated explanations
Example:
A provider begins a prior authorization request online but pauses before uploading documentation.
When they later contact support, the AI retrieves the incomplete case, confirms pending requirements, and resumes submission without restarting the process.
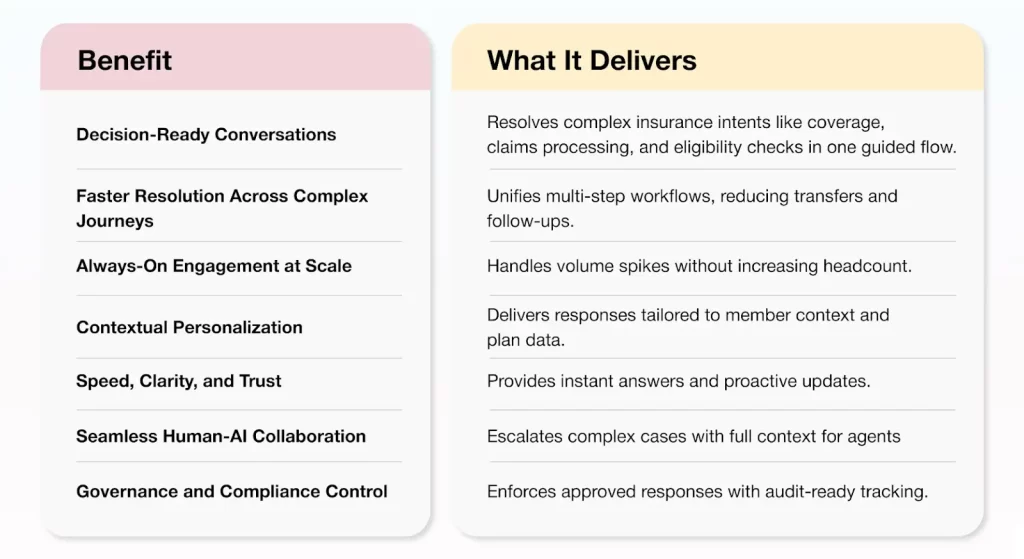
The Real Benefits of Conversational AI for Healthcare Insurers in 2026
When implemented correctly, conversational AI delivers value far beyond call deflection. It changes how insurers resolve intent, scale service, and build trust without increasing operational burden.
Here are the benefits that matter most to healthcare insurers.
A Step-by-Step Roadmap for Adopting Conversational AI in Insurance
Adopting conversational AI requires a well-defined strategy. Here’s how insurers can make the transition:
Step 1: Define Clear Objectives and KPIs
Anchor goals to metrics like cost-to-serve reduction, first-contact resolution, and CSAT rate.
Step 2: Assess Data and Technology Readiness
Ensure your data is clean and your systems are ready to integrate with conversational AI platforms.
Step 3: Embed Governance, Compliance, and Guardrails
Check that your AI solution complies with healthcare regulations and is in line with the internal policies of the company.

Step 4: Run a Focused Pilot
Deploy conversational AI first for internal users to test accuracy, integrations, and compliance controls. Then extend to external stakeholders in controlled use cases before scaling to more complex, high-impact insurance processes.
Step 5: Choose the Right Partner
Partner with a trusted provider like AVIZVA, which offers proven expertise in healthcare insurance and AI technology.
Step 6: Iterate, Optimize, and Expand Use Cases
After the pilot is successful, double down on conversational AI across the various departments in your organization.
Step 7: Operationalize Across the Organization
Make conversational AI an integral part of your operations that not only supports your business but also works in harmony with your long-term strategic goals.
What Future-Ready Conversational AI Looks Like in 2026—with VIZCare AI

Healthcare insurance conversations are getting more complex and patience is getting shorter. Members, brokers, employers, and providers want answers quickly, in plain language, without navigating portals or calling support.
That’s why conversational AI is rising fast in 2026. Insurers are adopting AI that can understand real insurance questions, maintain context, and take action; not just chat.
Solutions like AVIZVA’s VIZCare AI are driving this shift by turning conversations into a smarter, more reliable way to deliver insurance experiences. Let’s see how:
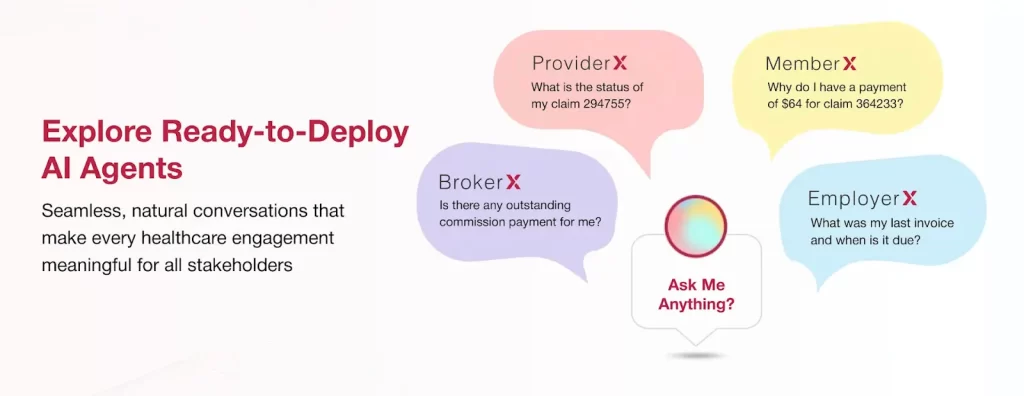
- Ready-to-Use Conversational Agents
Insurers no longer want to build conversational AI from scratch. Unlike generic conversational tools, VIZCare AI delivers production-ready AI agents designed specifically for insurance operations.
These agents don’t just answer questions, they deliver prebuilt intelligence that understands intent, retains context, and supports end-to-end insurance workflows from day one.
What this looks like in practice
- Service & Operations Agents
Support service teams during live interactions with intent detection, intelligent call summaries, and real-time guidance. Automated after-call actions reduce manual effort while improving accuracy and continuity.
- Broker Agents
Enable brokers to generate quotes, compare plans, understand commissions, and manage onboarding through conversational commands. This turns complex sales and post-sales processes into guided, actionable flows. - Employer Agents
Help employers manage enrollments, invoices, payments, and employee updates through simple conversations. This removes dependency on forms, tickets, and repeated follow-ups. - Member Agents
Translate benefits, coverage, claims, and payments into clear, plain-language interactions. Members are guided through updates, submissions, and next steps without friction or confusion.
- Provider-Facing Agents
Streamline eligibility checks, prior authorization requirements, claims guidance, and financial clarity. Conversational access to critical information helps reduce administrative delays.
- Conversations That Actually Understand Healthcare Insurance
Healthcare insurance conversations are complex. Members don’t ask simple questions; they ask situational, multi-layered questions involving plans, coverage rules, claim details, and demographic updates, etc.
Generic conversational tools struggle here. Insurance requires domain-specific intelligence built into the conversation layer.
What makes the difference:
- Healthcare insurance–trained intelligence, not generic language models.
- Built-in understanding of claims, benefits, eligibility, authorizations, and payer workflows.
- Enables seamless workflow coordination that adapts as conversations evolve without resetting or breaking logic.
This is where solutions like VIZCare AI move beyond conversational interfaces and become operational infrastructure for insurance workflows.
- Trust, Privacy, and Compliance Are No Longer Optional:
Conversational AI only scales in healthcare insurance when security and compliance are built in, not bolted on. What insurers expect in 2026:
- HIPAA, SOC 2, GDPR-aligned architectures.
- Private deployments with full data control.
- No model training on sensitive member data.
What’s changed is simple: today’s conversational AI is designed to give reliable answers based on the right data and only to the people who should see it.
VIZCare AI gives insurers a proven conversational foundation, while AVIZVA’s healthcare engineering teams help tailor it to real business workflows, systems, and stakeholder needs. The result is AI that works in production, not just in demos.

Final Thoughts
Conversational AI is no longer an experience add-on for healthcare insurers. It has become a servicing strategy, a data activation layer, and a competitive differentiator.
The real question is no longer if insurers should adopt conversational AI, but how deeply it is embedded across the service lifecycle—from enrollment and coverage clarity to compliance, and ongoing engagement.
See what enterprise-grade conversational AI looks like in practice.
Get in touch with us and see how VIZCare AI helps insurers move from chatbot experiments to enterprise-ready conversational AI.

FAQs
1. What are the main benefits of conversational AI for insurers?
Conversational AI helps insurers modernize service operations while maintaining control over costs and complexity. Key advantages include:
- Reduced servicing overhead by handling frequent, repeat interactions digitally.
- Faster resolution of complex workflows such as claims, eligibility, billing, onboarding, and renewals.
- Consistent, policy-aligned communication that reduces confusion and administrative friction.
- Scalable engagement during peak periods without increasing headcount.
- Built-in governance and compliance controls that ensure secure, audit-ready interactions across channels.
2. Why are healthcare insurers adopting conversational AI in 2026?
Healthcare insurers are increasingly seeing higher processing volumes, ever-escalating policy complexity, and vastly greater needs for speed and clarity. Conversational AI is built to meet these challenges, which include:
- Handling routine and semi-complex interactions at scale.
- Reducing dependency on manual support teams.
- Delivering consistent responses across channels.
- Unlocking enterprise data for real-time conversations.
3. How does conversational AI improve member experience in health insurance?
Conversational AI improves member experience by making insurance interactions simpler and more connected. It enables:
- Plain-language explanations of coverage and benefits.
- Real-time updates instead of delayed callbacks.
- Continuity across conversations and channels.
- Fewer handoffs and less repetition.
Members get faster answers, clearer guidance, and smoother journeys—without navigating multiple systems.
4. What are common mistakes insurers make when adopting conversational AI?
Many insurers struggle because they treat conversational AI as a chatbot rather than an enterprise capability. Common mistakes include:
- Deploying AI without a clear integration strategy aligned to the intended use cases and system landscape.
- Focusing only on FAQ deflection instead of intent resolution.
- Ignoring governance, compliance, and escalation rules.
- Launching pilots without clear success metrics.
- Failing to integrate AI into day-to-day operations.
5. Is conversational AI secure for healthcare insurance data?
Yes, conversational AI can be secure for healthcare insurance data, but security is not automatic. It depends on deploying enterprise-grade, compliant solutions tailored to insurance environments. Solutions like VIZCare AI are built to meet regulatory requirements and handle sensitive insurance data securely and responsibly.

