Table of Contents
Key Takeaways
- The Dilemma: Most members are dissatisfied and demand more personalized insurance experiences
- The Shift: Move from reactive “black boxes” to proactive, insurance AI solutions.
- VIZCare Advantage: Power portals like MemberX with real-time, context-aware intelligence.
- Bottom Line: Turn member support from a cost burden into a strategic loyalty engine.
For most members, their relationship with their health insurer is surprisingly minimal. Outside of paying premiums or checking on a claim, interactions are rare and often frustrating. When questions arise about coverage, benefits or claims status, members frequently encounter long wait times, understanding complex policy documents or limited visibility into what’s actually happening behind the scenes. To many consumers, health insurance still feels like a black box, quite most of the time and confusing when they really need it.
At the same time, expectations have changed dramatically. Today’s healthcare consumers are accustomed to real-time answers, personalized recommendations, and seamless digital experiences in almost every other aspect of their lives. Recent industry data shows that only 45% of healthcare consumers are fully satisfied with their health insurance, while 55% expect more personalized engagement from their health plans.
This widening gap between what members expect and what insurers can realistically deliver is beginning to show operational strain. Contact centers are overwhelmed, service teams face rising interaction volumes, and member experience delays that erode trust over time.
To address this challenge, many organizations are turning to insurance AI solutions. By combining conversational AI, intelligent automation, and real-time data access, these technologies are helping insurers close the engagement gap delivering faster support, reducing service fatigue, and enabling more personalized member interaction at scale.
In this blog, we explore how AI solutions for healthcare insurers are transforming member engagement making insurance more transparent, responsive, and easier to navigate for the people who rely on it most.
The Trust Gap: Why Current Support Models Fall Short
Closing the trust gap requires a move toward insurance AI solutions that prioritize transparency. With AI solutions designed for healthcare member support, insurers can move from deflecting calls to resolving member intents.
The trust gap emerges when members feel disconnected from their insurer often during the very moments when they need clarity the most. Long wait times, unclear explanations, and inconsistent answers across channels create frustration and uncertainty. Instead of receiving proactive guidance, members are often left chasing information themselves.
Common signals of the trust gap include:
- Repeating the same issue across multiple channels
- Delays in understanding coverage or claim explanations or decisions
- Inconsistent answers from different support representatives
- Overloaded service teams handling high interaction volumes
- Limited visibility into the next steps in a member’s journey
Bridging the Gap with Insurance AI Solutions
Closing this gap requires a shift from reactive service models to intelligent, proactive engagement. Modern insurance AI solutions empower insurers to go beyond call deflection; resolving member needs instantly with intelligent, context-aware support.
By combining conversational AI, real-time data access, and intelligent workflows, these solutions provide members with clear answers, consistent information, and guided next steps helping insurers deliver more transparent, responsive, and scalable support experiences.
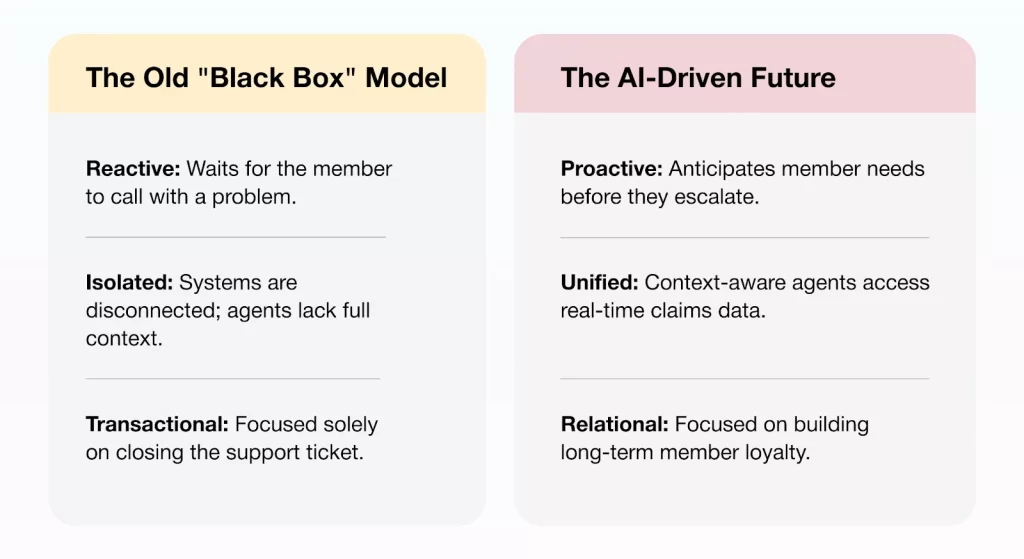
Tackling Support Fatigue: How AI Automation Fixes Broken Member Experiences
Support fatigue is becoming a growing challenge for healthcare insurers. As member inquiries continue to rise, contact centers are overwhelmed with routine questions like coverage checks, claim status updates and eligibility confirmations leaving little room for agents to focus on complex or high-value interactions.
When service teams spend most of their time answering questions like “Has my claim been processed?” or What’s the status of my claim?” their ability to handle nuanced member concerns inevitably declines. Over time, this creates operational strain and a poorer experience for members.
The Impact of Support Fatigue:
- Member Dissatisfaction: Long wait times and unresolved queries erode trust and satisfaction
- Increased Operational Costs: High call volumes require more staffing and resources to manage
- Agent Burnout: Continuous pressure from repetitive queries reduces productivity and increases turnover
How AI Automation Reduces Support Fatigue
AI automation helps insurers break this cycle by shifting repetitive tasks away from human teams while maintaining service quality.
- Automating routine interactions: AI assistants can instantly resolve common queries such as claim status, eligibility checks, and coverage details etc., reducing inbound call volume and freeing agents to focus on sensitive or complex cases.
- Continuous support availability: AI-powered virtual assistants provide 24/7 support across digital channels, allowing members to get answers anytime without increasing staffing requirements
- Proactive, AI-driven communication: Instead of waiting for members to reach out , AI can trigger automated reminders, update on claims, and send notifications on next-step alerts preventing unnecessary follow-ups.
By reducing routine workload and enabling proactive engagement, AI allows service teams to focus on what matters most: delivering meaningful support when members truly need it.

Personalizing Member Engagement : The Power of AI-Driven Insights
In the era of 1-to-1 digital experiences, generic “Dear Member” communications are the fastest way to lose trust. Healthcare Insurers face a difficult challenge, i.e., delivering personalized engagement to millions of members while keeping operational costs under control. AI-driven insights help close this gap by enabling meaningful personalization at scale without adding administrative complexity.
How Data-Driven AI Personalization Helps
AI-powered solutions such as AVIZVA’s VIZCare AI transform member engagement by turning vast volumes of data into real-time, actionable insights.
Leveraging Member Data Intelligently
AI analyzes large datasets including member history, coverage details, preferences and past interactions to tailor each engagement. This ensures every response is relevant, contextual and aligned with the members’ unique situation.
Human-like Conversational Interactions
Modern AI agents in healthcare use natural language processing (NLP) and machine learning to engage in intuitive conversations. This allows them to:
- Provide clear, context-aware answers to complex questions
- Recommend plans or services based on member needs and history
- Explain insurance processes in simple, easy-to-understand language
Consistent omnichannel engagement
With shared context across channels, AI ensures members receive consistent support whether they interact through phone, mobile apps, or web portals. This creates a seamless experience that feels connected and continuous, strengthening member satisfaction.
Let’s take an example : Imagine a member calling to ask about coverage for a specific procedure. After waiting on hold, they reach a representative who lacks full context. The member must repeat details, explain their situation again, and navigate unclear answers, an experience that quickly leads to frustration.
With VIZCare AI :
- The AI agent instantly accesses the member’s coverage and policy information to provide the right response without needing to navigate the hassle of going through the entire documentation
- Conversation history and context are retained automatically, eliminating repetition
- If human support is required, the interaction is seamlessly transferred to an agent with the full context of the conversation, saving time for both the member and the support agent.
By combining data intelligence with conversational AI, insurers can move beyond generic communication to deliver personalized, responsive, and efficient member engagement at scale.
Three Moves Insurers Must Make to Modernize Member Engagement
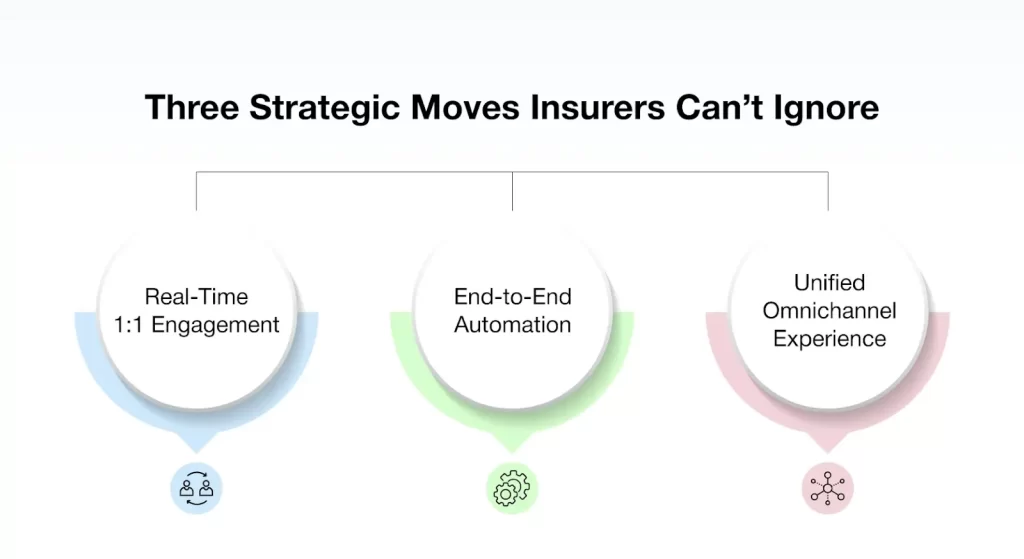
Modernizing member engagement isn’t about adding more channels or tools, it’s about building core capabilities that allow insurers to respond intelligently, act quickly, and maintain consistency across every interaction.
Here are three critical moves insurers must make to transform the healthcare member experience:
1. Enable 1-to-1 Engagement with Real-Time AI
Effective engagement depends on relevance at the moment. Members expect insurers to instantly understand who they are, what plan they have, and why they’re reaching out instantly,
Real-time AI-enabled tools, such as VIZCare AI, make this possible by combining intent recognition, contextual access to plan and policy data, and conversational AI agents. These agents interpret the member’s request, retrieve the right information instantly and deliver personalized guidance ensuring consistent resolution across channels.
2. Connect the Front and Back Office with End-to-End Automation
True engagement transformation requires bridging the gap between customer-facing teams and operational teams.
By integrating AI and automation into back-office workflows, insurers can resolve routine tasks such as address changes, mail documents or ID Cards without human intervention. This eliminates the “we’ll get back to you” delivery approach that erodes member trust.
3. Deliver A Unified Omnichannel Experience
Members interact with insurers through multiple touchpoints such as web portals, mobile apps, emails, and messaging platforms. These experiences must feel seamless and connected.
AI-powered engagement platforms maintain shared context across channels, ensuring members receive consistent responses regardless of how they interact. This creates a unified, continuous experience that improves satisfaction and reduces service friction.
Turning Member Support into a Strategic Advantage with AVIZVA’s AI-Driven Solutions
To thrive in the competitive health insurance landscape, organizations must transition from being “claim payers” to becoming “experience partners.”
This transformation is realized through the VIZCare Xperience platform, specifically through the MemberX portal, a unified experience layer designed to put the member at the center of the healthcare journey.
MemberX: Where Support Becomes Simpler and More Intuitive
MemberX is designed around how members actually seek information, not how systems store it. Instead of navigating portals, documents, and forms, members interact through a single, guided experience.
Through MemberX, members can:
- Access profile details, benefits, and coverage information in one place
- Understand plan details and EOBs in clear, plain language
- View claim status, payments, and pending actions without confusion
- Update personal or contact information conversationally
- Complete claim-related actions with step-by-step guidance
Each interaction is designed to reduce friction, prevent follow-ups, and give members clarity in the moment without increasing service load.
Intelligence That Powers Every Interaction
What makes MemberX effective is not just the interface, but the intelligence behind it.
VIZCare AI-driven intelligence powers MemberX by continuously interpreting intent, retaining context, and pulling the right information at the right time. AI agents work alongside automation and rules to ensure conversations don’t stop at answers they lead to action.
This intelligence enables:
- Context-aware responses across channels
- Real-time access to plan and claim data
- Automated actions triggered during conversations
- Seamless escalation with full interaction history
Instead of treating support as isolated transactions, insurers gain a connected engagement layer that scales, stays compliant, and adapts as member needs change.
1. Extending Intelligence Beyond Member Support
While MemberX plays a critical role in member engagement, VIZCare AI is the intelligence layer that powers experiences across the entire insurance ecosystem. Here are some of the features offered by the platform:
2. Deep Healthcare Insurance Intelligence
VIZCare AI is built with deep, domain-specific knowledge of healthcare insurance, enabling it to understand complex member queries and deliver accurate, context-aware answers. It simplifies policy terms, guides members through plan benefits and claims, and offers proactive suggestions all in natural language. This intelligence enhances self-service and boosts member confidence in navigating their coverage.
3. Private, Secure, and Compliant by Design
Designed with enterprise-grade privacy and compliance at its core, VIZCare AI ensures all member data stays protected within the insurer’s infrastructure. It meets HIPAA, SOC 2, and GDPR standards, giving members the confidence to engage with sensitive insurance tasks securely. This trust-first approach encourages greater use of digital tools and increases overall satisfaction.
4. Member Agents Offering Full Functional Coverage
VIZCare AI doesn’t just answer questions, it gets things done. Through its agentic design, members can complete tasks like updating personal info, submitting claims, or retrieving documents right within the conversation. This seamless, action-oriented experience reduces effort and strengthens engagement through instant, personalized service.
5. Guaranteed Data Accuracy
With robust access control, VIZCare AI ensures members see only the information relevant to them and that it’s always accurate. Whether it’s claim status or benefit details, the AI pulls verified data in real-time, eliminating confusion or misinformation. This builds data trust and reinforces confidence in every interaction.
Moreover, it combines conversational AI, real-time data access, workflow automation, and custom AI applications to support both external stakeholders and internal teams. Insurers can deploy pre-built AI agents or create custom AI apps tailored to specific business workflows ensuring every interaction is context-aware, secure, and consistent.
Built on a shared intelligence foundation, VIZCare AI supports multiple stakeholder journeys through purpose-built AI agents and applications, including:
- Broker Agents: Guide quoting, plan comparisons, and commission-related inquiries through conversational workflows.
- Provider Agents: Deliver real-time clarity on eligibility, claim status, and authorizations.
- Employer Agents: Simplify enrollment, billing, and benefits administration through AI-assisted interactions.
- Service & Operations Agents: Support internal teams with real-time guidance, call summaries, and automated follow-ups.
Because every AI agent and portal shares context and intelligence, interactions remain consistent as users move across channels, departments, and roles. This allows insurers to modernize engagement holistically without creating disconnected experiences or duplicating effort.

How to Implement AI-Driven Solutions in Your Insurance Organization
Implementing AI-driven solutions can seem like a monumental task. However, with the right approach, insurers can successfully integrate AI into their operations, improving both efficiency and member engagement.
Here’s a step-by-step guide to ensure smooth implementation:
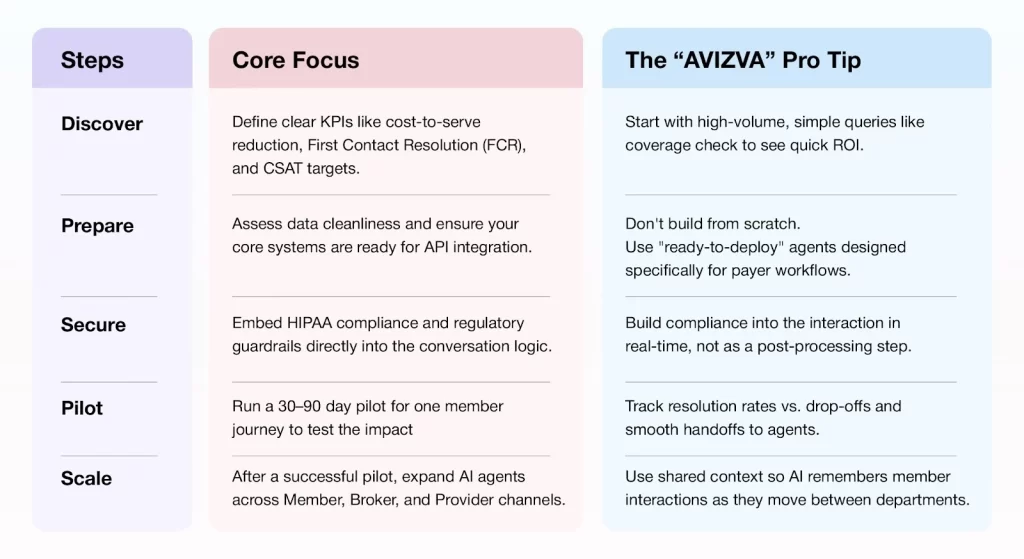

Conclusion
As we look forward, switching to AI solutions in the insurance sector is certainly more a question of “how fast” rather than “if”.
Healthcare insurance powered by AI opens up an obvious direction for the future. By closing the trust gap, reducing support fatigue, and enabling personalized engagement at scale, insurers can boost efficiency without compromising compliance or experience.
Prepared with the proper approach and a healthcare-capable ally like AVIZVA, member support can transform from being a cost center to becoming a sustainable competitive advantage.
Ready to modernize member engagement? Contact AVIZVA and explore how its AI-driven solutions can help you close the trust gap and scale smarter support.

FAQs
1. How can AI improve member support and engagement in healthcare insurance?
AI enables insurers to respond more quickly, provide clearer information, and thus reduce the number of repeat contacts. It handles routine inquiries, maintains conversation history, and enables cross-channel, consistent engagement leading to higher customer satisfaction while lowering cost-to-serve.
2. What types of member support tasks can be automated with AI in healthcare insurance?
AI solutions for insurance are designed to handle high-volume, repetitive administrative inquiries that typically overwhelm call center agents:
- 360° Healthcare Access: Getting all members, coverage, and plan details at once without multiple steps.
- Simple Plan Explanations: The AI “translates” complex insurance terms and plan documents into clear, everyday language so members know exactly what is covered.
- Eligibility & Benefits: Instantly clarifying coverage limits and out-of-pocket costs.
- Claim Status Checks: Providing real-time status updates and guided submission steps.
- Instant Information Updates: Members can update their address, contact info, or personal details instantly during a chat without filling out forms.
3. How do AI-powered chatbots and virtual assistants help health plan members?
AI-powered chatbots and virtual assistants explain coverage, benefits, and policy terms in simple, easy-to-understand language while retaining conversation context across channels. This allows members to move from mobile apps to web portals without having to start over.
Unlike basic rule-based chatbots, these AI assistants can interpret the purpose of a query, maintain conversation history across interactions, and intelligently escalate complex cases to human agents with full context when needed.
4. Can insurance AI solutions handle complex member questions, or are human agents still needed?
Yes, insurance AI solutions can handle many complex member questions by accessing real-time plan and policy information. However, human agents are still needed for situations that require judgment or empathy. In these cases, conversational AI supports human agents by sharing conversation context and key details, so issues are resolved faster.
5. What are the benefits of using AI to automate member engagement for insurers?
Implementing AI for healthcare insurers scales the organization’s capacity while significantly improving operational metrics:
- Cost Reduction: Lowers servicing overhead through digital intent resolution.
- Improved Retention: Higher satisfaction scores (CSAT) driven by faster, more accurate responses.
- Regulatory Control: Enforces compliance across all interactions.

